Revenue Cycle Management Services
Revenue Cycle Management Services that help healthcare providers manage billing, claims and payments so your practice keeps a steady cash…


Explore services to learn more
MedicalBilling Help provides Denial Management Services for clinics and healthcare providers. Our team reviews your denied claims, finds the reasons, fixes billing or coding issues and sends clear appeals. We work each claim until we get an answer so you recover more revenue, reduce write offs and keep your cash flow steady while you focus on patient care.
Our mission is to make Denial Management Services simple and clear for healthcare providers. We help you understand why claims deny, correct the problems and turn unpaid claims into payments so you see more of the money you earn.
Our objective is to be the trusted choice for Denial Management Services in USA. We support every client with honest guidance, steady follow up and a friendly team that understands how hard you work to care for your patients.
Claims . Denials . Review . Appeals . Approval . Recovery
Revenue Cycle Management Services that help healthcare providers manage billing, claims and payments so your practice keeps a steady cash…
Revenue Cycle Management Services that help healthcare providers manage billing, claims and payments so your practice keeps a steady cash flow.
We accurately post ERAs/EOBs, reconcile payments, identify underpayments, and keep your reports clean so you can focus on patient care…
We accurately post ERAs/EOBs, reconcile payments, identify underpayments, and keep your reports clean so you can focus on patient care while we protect your cash flow.
Medical Credentialing Services for healthcare providers, making insurance enrollment simple and faster.
Medical Credentialing Services for healthcare providers, making insurance enrollment simple and faster.
MedicalBilling Help offers Medical Coding Services in USA for healthcare providers. Our team handles accurate coding and clean claims so…
MedicalBilling Help offers Medical Coding Services in USA for healthcare providers. Our team handles accurate coding and clean claims so your practice gets paid on time.
Reliable billing that improves collections month after month.
Reliable billing that improves collections month after month.
Insurance Eligibility Verification Services that check patient coverage and benefits in advance so your practice avoids surprise denials and keeps…
Insurance Eligibility Verification Services that check patient coverage and benefits in advance so your practice avoids surprise denials and keeps cash flow steady.
MedicalBilling Help is a trusted partner for Denial Management Services. We support healthcare providers across the USA by reviewing denied claims, finding the reason for each denial and sending clear corrections and appeals. You save staff time, reduce write offs and protect your revenue when you trust us with your denial work.
Our denial management team reviews each denied claim with care so payers receive clear and correct information.
We protect patient data and follow every privacy rule and guideline in our daily work.
We manage high volumes of denied claims and follow ups for busy clinics and healthcare providers across the USA.
Many providers across the USA rely on our Denial Management Services to recover revenue and keep cash flow steady.
Denial Management Services review denied claims, find the reasons for the denial and correct billing or coding issues so the claim can be paid. This helps healthcare providers recover revenue that might otherwise turn into write offs.
Healthcare providers use Claim Denial Management Services to cut down on lost payments, avoid long follow up work and make sure every denied claim receives proper review, correction and appeal.
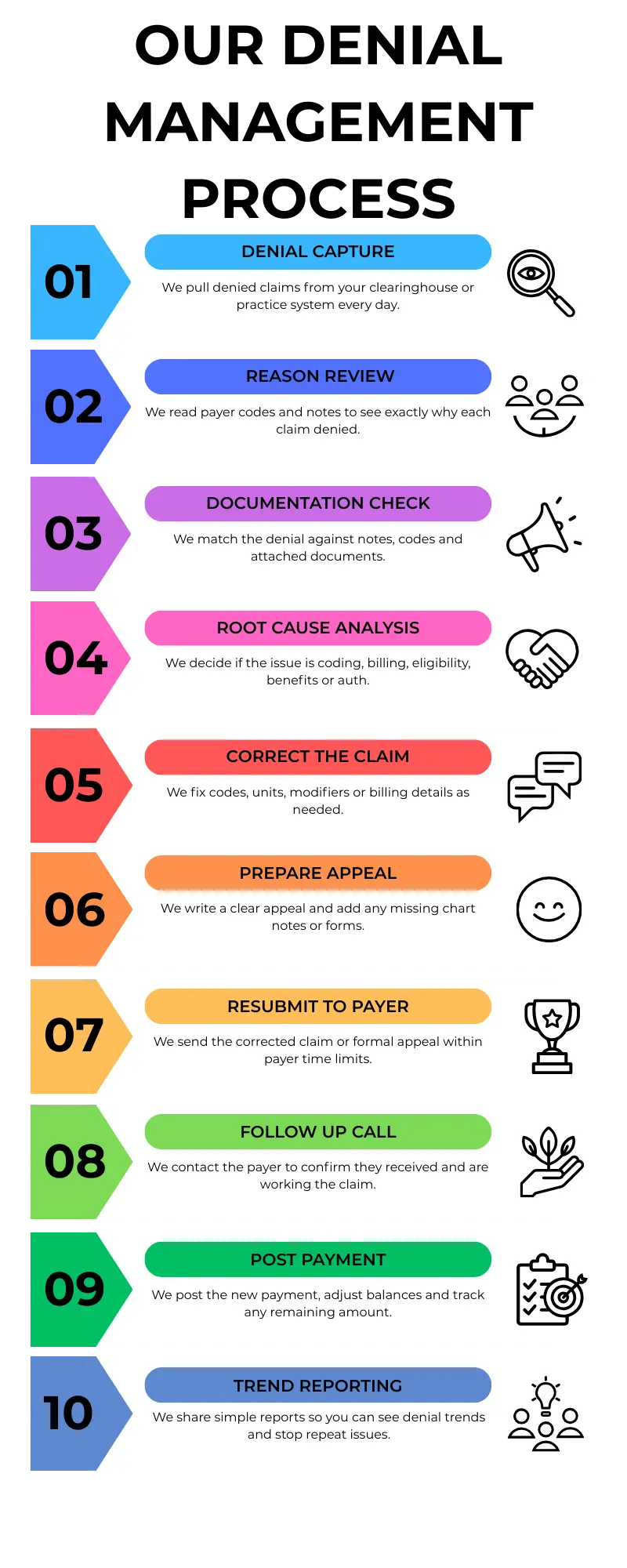
Our Denial Management Services in USA follow a clear process: we review the denial, check the payer rules, fix errors and send a clean appeal. We continue follow up until we receive a final payer response.
Our Denial Management and Appeals process includes denial review, coding and billing correction, appeal letter preparation, document submission and continuous follow up until the claim is fully resolved.
Our Denial Management Services for Healthcare Providers handle complex review and appeal steps so your team can stay focused on patient care instead of paperwork and long payer calls.
Yes. We provide full AR and Denial Management Services, including aging follow up, denial tracking, appeal management and reporting to help your clinic maintain steady cash flow.
Yes. We work with commercial payers, Medicare, Medicaid and specialty plans, ensuring every denied claim is reviewed and sent with the correct appeal.
NEED GUIDANCE ON MEDICAL BILLING? WE’RE HERE TO TALK.
© 2026 Medical Billing Help. All Rights Reserved.