Revenue Cycle Management Services
Revenue Cycle Management Services that help healthcare providers manage billing, claims and payments so your practice keeps a steady cash…



Explore services to learn more
MedicalBilling Help provides Medical Credentialing Services for clinics and healthcare providers. Our team works as a Professional Medical Credentialing Company that collects your documents, completes payer forms and follows up until approval. With our Outsourced Medical Credentialing Services you join insurance networks faster and spend more time with your patients instead of paperwork.
Our mission is to make Medical Credentialing Services simple and clear for healthcare providers. We help you keep licenses, enrollments and payer records accurate so your practice stays ready to see patients and receive payment.
Our objective is to be the trusted Professional Medical Credentialing Company in USA. We aim to support every client with honest guidance, steady updates and a helpful credentialing team that understands how providers work.
Providers . Credentialing . Support . Payer . Enrollment . Updates
Revenue Cycle Management Services that help healthcare providers manage billing, claims and payments so your practice keeps a steady cash…
Revenue Cycle Management Services that help healthcare providers manage billing, claims and payments so your practice keeps a steady cash flow.
We accurately post ERAs/EOBs, reconcile payments, identify underpayments, and keep your reports clean so you can focus on patient care…
We accurately post ERAs/EOBs, reconcile payments, identify underpayments, and keep your reports clean so you can focus on patient care while we protect your cash flow.
MedicalBilling Help offers Medical Coding Services in USA for healthcare providers. Our team handles accurate coding and clean claims so…
MedicalBilling Help offers Medical Coding Services in USA for healthcare providers. Our team handles accurate coding and clean claims so your practice gets paid on time.
Reliable billing that improves collections month after month.
Reliable billing that improves collections month after month.
Insurance Eligibility Verification Services that check patient coverage and benefits in advance so your practice avoids surprise denials and keeps…
Insurance Eligibility Verification Services that check patient coverage and benefits in advance so your practice avoids surprise denials and keeps cash flow steady.
Denial Management Services that review denied claims, manage appeals and help healthcare providers recover revenue that might otherwise turn into…
Denial Management Services that review denied claims, manage appeals and help healthcare providers recover revenue that might otherwise turn into write offs.
MedicalBilling Help is a professional medical credentialing company that supports healthcare providers across the USA. Our team delivers accurate Medical Credentialing Services, gathers every document with care and works with payers until approval. You save staff time, avoid delays and protect your revenue when you trust us with your credentialing work.
Our medical credentialing team sends complete and accurate files so payers approve providers faster.
We protect patient and provider data and follow every privacy rule and guideline.
We manage high volumes of forms, updates and enrollments for busy clinics and healthcare providers.
Many providers across the USA rely on our Medical Credentialing Services to stay in network and ready to see patients.
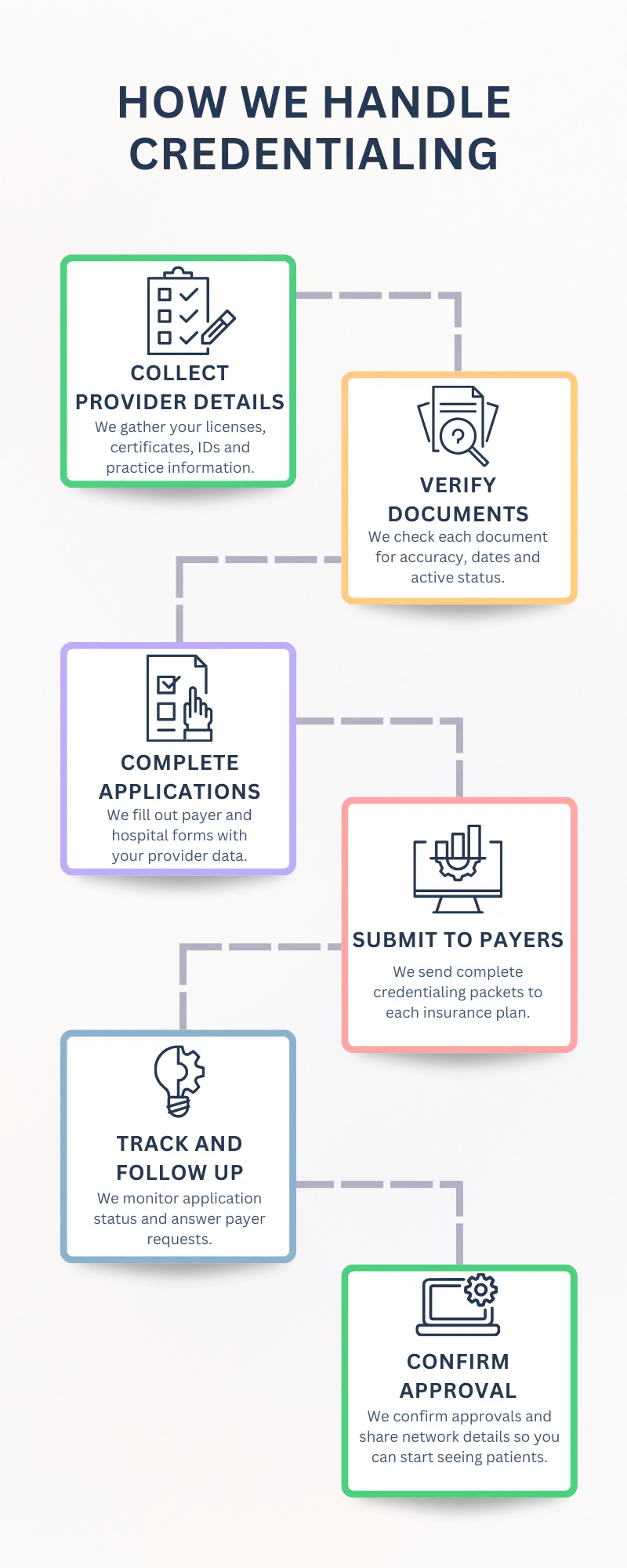
Our Medical Credentialing Services include collecting your provider documents, checking licenses, filling payer forms and tracking every application. We manage these steps for you so your practice stays ready to see patients and receive payment.
Our Medical Credentialing Services in USA help your practice stay active with major insurance plans. We follow payer rules, watch deadlines and keep your records current so your providers avoid gaps in coverage.
When you work with our Professional Medical Credentialing Company, you get a team that handles credentialing every day and knows what payers expect. We reduce mistakes, follow up with each plan and free your staff from long calls and paperwork.
Our Provider Credentialing Services support your doctors, nurses and other licensed providers who need to join or stay in insurance networks. We set up new providers, update existing ones and handle changes when your team moves locations or adds a new tax ID.
Our Outsourced Medical Credentialing Services fit around your current office team. Your staff shares basic provider details and we handle payer forms, document updates and follow ups. We keep your team updated on every application so they stay informed without spending hours on credentialing work.
Our Medical Credentialing for Healthcare Providers makes sure your providers are approved and in network with payers. When credentialing is complete and accurate, your claims have a better chance of being paid on time and at the right rate.
NEED GUIDANCE ON MEDICAL BILLING? WE’RE HERE TO TALK.
© 2026 Medical Billing Help. All Rights Reserved.