Medical billing has many steps, and each step helps a claim reach the correct place. One important part of this process is the ICN number in medical billing. Many people hear this term but do not fully understand what it means.
The ICN number helps clinics, billing teams, and insurance companies track claims and solve problems with ease. When you learn how the ICN number in medical billing works, you gain better control over the entire payment process.
The ICN number works like a tracking code. It helps you follow a claim from the moment the insurance company receives it until the moment they release payment.
This guide explains what the ICN number in medical billing means, where to find it, how it works, and why it matters to every practice.
Table of Contents
ToggleWhat the ICN number in medical billing means?
The ICN number in medical billing stands for Internal Control Number. Some payers also call it the “Claim Control Number”.
When the insurance company receives a claim, their system creates this number right away. The ICN number becomes the unique fingerprint of the claim. Every claim has its own ICN number, and this number never matches another claim.
This number helps the payer track the claim inside their system. It gives them a simple way to find the claim when you call, send an appeal, or ask for a review.
Without the ICN number, a payer would have a hard time searching through millions of claims each year.
Where to find the ICN number?
You can find the ICN number in several places. It appears on the Explanation of Benefits, the Electronic Remittance Advice, and inside the payer portal. Many billing programs also save the ICN number after the payer sends the first response.
| Source | How it appears | What it helps you do |
|---|---|---|
| Explanation of Benefits | ICN or Claim Control Number on the remit line | Match payment to the claim |
| Electronic Remittance Advice | ICN shown in payment details | Confirm status and codes |
| Payer Portal | ICN listed in claim view | Check claim progress |
| Billing Software | Imported after first payer reply | Track the claim in your system |
How the ICN number in medical billing helps payers?
Insurance companies use the ICN number to organize and manage claims. When a claim enters their system, the ICN number becomes the main link for every update. It helps the payer track what they did with the claim, when they received it, and what the final result was.
If you call a payer and ask about a claim, they will ask for the ICN number first. Once they have it, they can pull up the claim in seconds. This saves time for both the payer and the billing team.
Why the ICN number in medical billing matters to billing teams
Billing teams use the ICN number every day. They use it to check claim status, solve issues, find unpaid claims, and work on denials. When a claim is denied, the ICN number becomes the most important detail. It tells the payer which claim you want them to reopen or review.
When you send a corrected claim or an appeal, the payer often requires the ICN number. It helps them connect the original claim with the new one. This keeps the claim record clean and prevents delays.
The ICN number also helps billing teams match payments with claims. When the number on the remit matches the number in the system, posting becomes simple and clear.
How the ICN number in medical billing helps providers?
Providers may not use the ICN number every day, but they still depend on it. When the billing team uses the ICN number to follow up fast, claims move through the system without delay. This means faster payments and fewer issues for the practice.
Providers often want to know when a claim will pay. If they give the billing team or payer the ICN number, they can get a clear update right away. This gives providers peace of mind and helps the practice stay organized.
How the ICN number reveals claim details
Some payers build meaning into the ICN number. The first part may show the year the payer received the claim. Another part may show the day of the year. Another part may show the claim type. This helps billing teams understand when the payer first touched the claim.
Not all payers follow this pattern, but many do.
How the ICN number helps with denied claims
Denied claims slow down payment and cause stress for staff. The ICN number in medical billing helps fix these problems. When a claim is denied, the billing team uses the ICN number to find it fast. They read the denial, make corrections, and send the claim again.
Appeals also depend on the ICN number. Without the correct ICN number, the payer may not know which claim you want them to review.
Charts that show how ICN tracking helps
Chart 1: Time to Payment by Stage
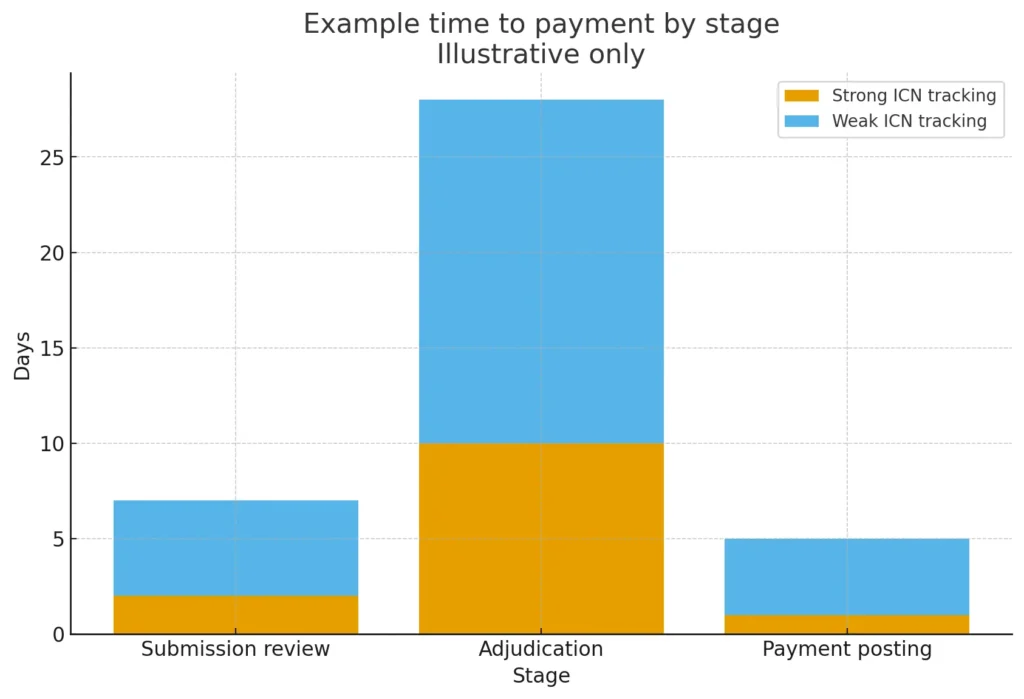
Chart 2: Paid Rate Over Time with Follow Up
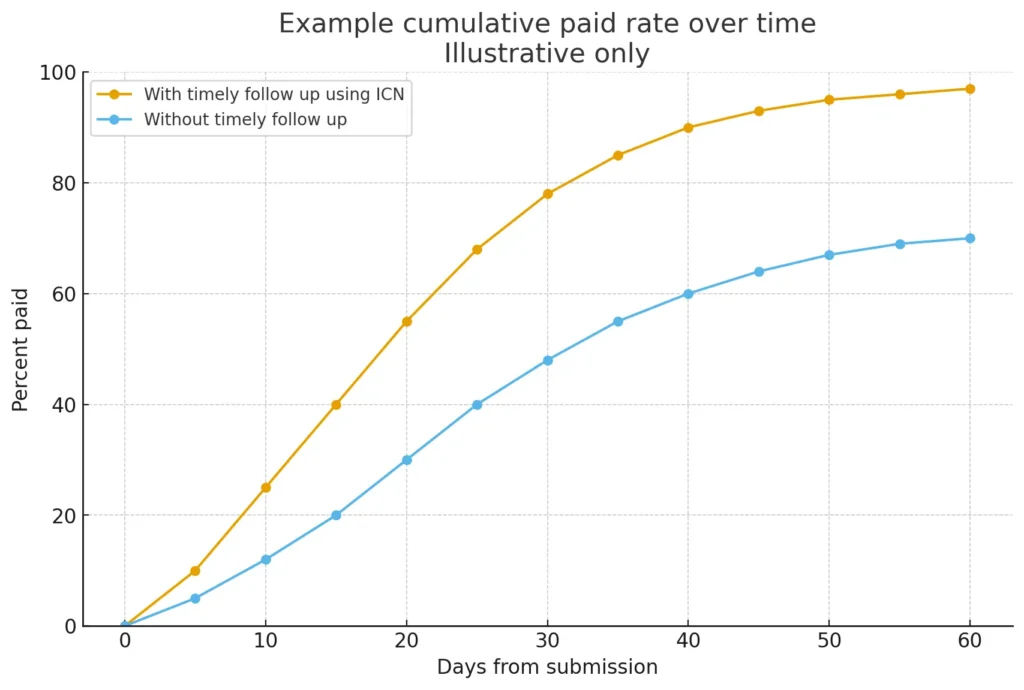
How the ICN number keeps records clean
Medical billing depends on clear records. The ICN number helps bring order to the entire revenue cycle. It reduces mix ups. It helps the billing team avoid duplicate claims. It allows clean posting and easy reporting.
When a practice uses the ICN number well, they can see which payers pay fast, which payers need follow up, and which claims need more care.
The ICN number in medical billing may look like a simple number, but it plays a major role in the entire claim journey. It helps clinics, billing teams, and payers stay organized. It helps solve denials. It helps track claims from start to finish. It supports clean records and faster payments.
When you understand the ICN number in medical billing and use it the right way, your practice becomes stronger, your claims move faster, and your revenue cycle becomes smooth and steady.
Stuck on an ICN problem or a delayed claim? Let Medical Billing Help fix it and keep your cash flow steady.




