If you run a mental health practice in the United States, you likely ask one key question again and again. How much does Blue Cross Blue Shield therapy reimbursement actually pay?
The answer is not simple. Blue Cross Blue Shield therapy reimbursement depends on many factors such as your contract, your location, the type of therapy session, and whether you are in network or out of network. Still, there are clear ranges and patterns that help you estimate your earnings and plan your billing strategy.
In this guide on medicalbilling.help, you will learn real numbers, how payments work, and how to increase your reimbursement.
Table of Contents
ToggleUnderstanding Blue Cross Blue Shield Therapy Reimbursement
Blue Cross Blue Shield therapy reimbursement means the payment you receive after you submit a claim for a therapy session. The insurance company reviews your claim and pays based on the allowed amount, not your billed amount.
The allowed amount is the rate that Blue Cross Blue Shield agrees to pay for a specific service. This amount is fixed through contracts if you are in network.
If you charge more than the allowed amount, you may not receive the difference. This is why understanding reimbursement is very important for your revenue.
Average Blue Cross Blue Shield Therapy Reimbursement Rates
Blue Cross Blue Shield therapy reimbursement usually falls within a predictable range depending on the session type. Below is a clear table showing average reimbursement ranges in the United States.
Therapy Reimbursement by CPT Code
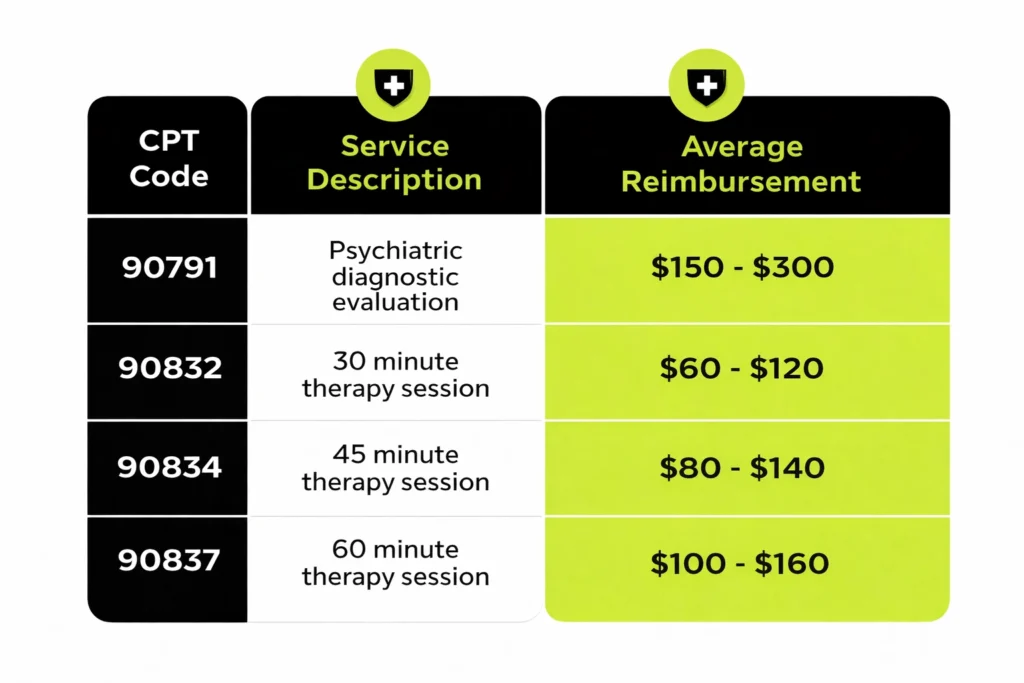
Across the US, many providers report an overall average reimbursement between about $72 and $102 for standard sessions.
These numbers are estimates, but they give a strong idea of what providers can expect.
How CPT Codes Affect Your Reimbursement
CPT codes play a major role in how much you get paid. Each therapy service has a specific code that tells the payer what service you performed.
For example, code 90834 represents a 45-minute therapy session, while 90837 represents a 60 minute session. The longer and more complex the session, the higher the reimbursement.
Insurance companies rely on these codes to process claims. If you use the wrong code, you may face delays or reduced payment.
Accurate coding is one of the most important parts of maximizing your therapy billing CPT codes usage and improving revenue.
In Network vs Out of Network Therapy Payments
Your network status can change your income significantly. Below is a simple comparison table to understand the difference.
In Network vs Out of Network Payments
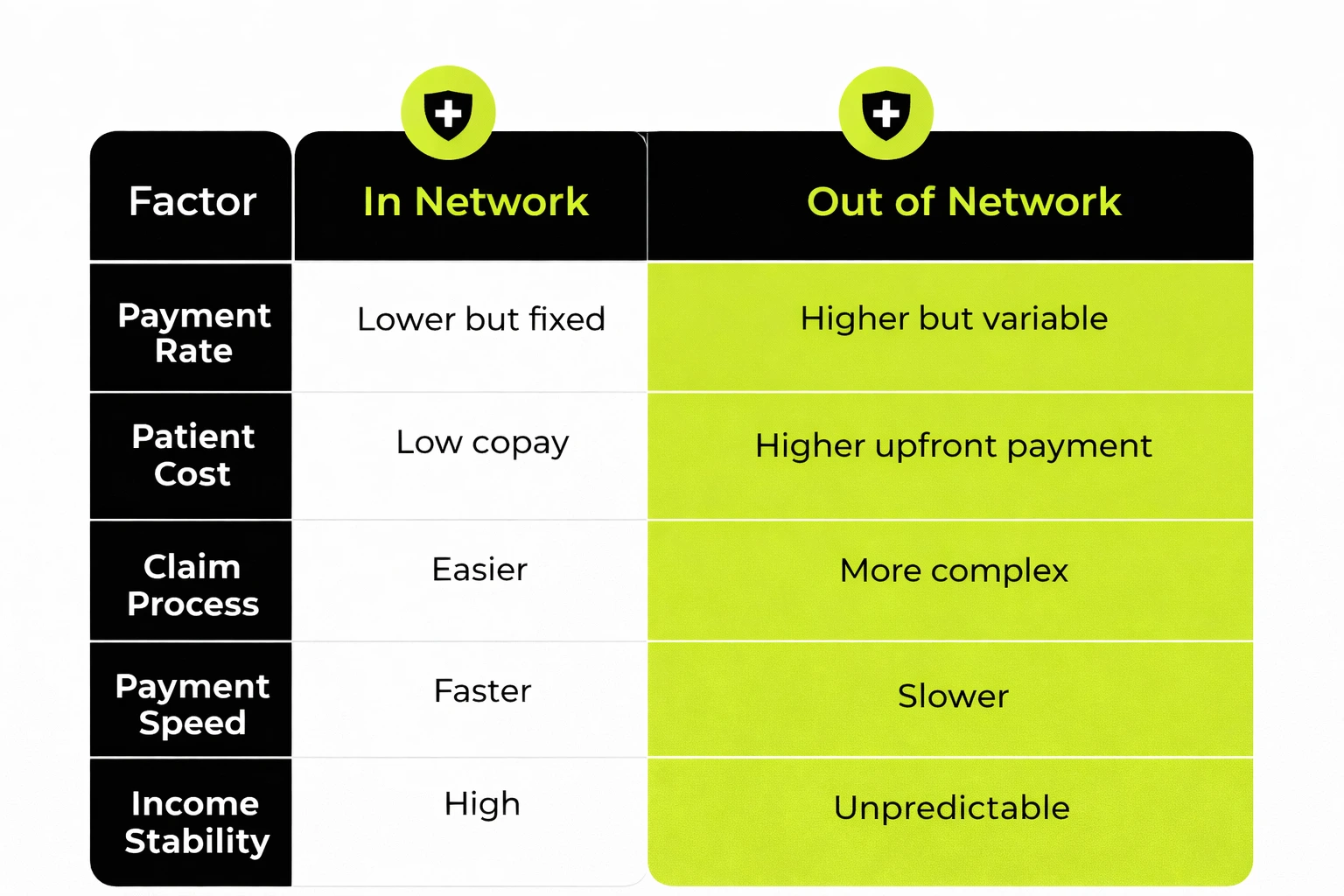
When you are in network, you agree to accept negotiated rates. These rates are lower than your full fee but offer steady payments and fewer claim issues.
When you are out of network, you can charge your full rate. However, reimbursement becomes less predictable, which is why many providers prefer in network vs out of network therapy balance carefully.
Factors That Impact Blue Cross Blue Shield Therapy Reimbursement
Blue Cross Blue Shield therapy reimbursement is not fixed. Many factors affect how much you earn.
Key Factors That Affect Reimbursement
Factor | Impact on Payment |
Location | Higher in urban areas |
Provider Credentials | Higher for psychologists and psychiatrists |
Type of Service | Specialized services pay more |
Contract Terms | Varies by BCBS state plan |
Billing Accuracy | Errors reduce payment |
Your location plays a major role. Providers in cities with higher living costs often receive higher payments.
Your credentials also matter. Licensed psychologists and psychiatrists often receive higher reimbursement than counselors or social workers.
The type of therapy also affects payment. Specialized services like crisis therapy or testing usually pay more than standard sessions.
How Blue Cross Blue Shield Plans Affect Therapy Payments
Not all Blue Cross Blue Shield plans offer the same coverage. Below is a table explaining common plan types.
BCBS Plan Types and Coverage
Plan Type | Coverage Style | Flexibility |
HMO | In network only | Low |
PPO | In and out of network | High |
EPO | In network only | Medium |
POS | Referral based | Medium |
Understanding plan types helps you explain costs to patients and reduce billing confusion.
Need Help Understanding BCBS Therapy Reimbursement?
Get clear support for therapy billing, claim submission, payment issues, and reimbursement questions.
Copays, Deductibles, and Coinsurance Explained
To fully understand Blue Cross Blue Shield therapy reimbursement, you must know how patient responsibility works.
Patient Cost Breakdown
Cost Type | Description | Typical Range |
Copay | Fixed amount per visit | $15 to $80 |
Deductible | Amount before coverage starts | $500 to $3000 |
Coinsurance | Percentage after deductible | 10% to 50% |
These factors directly affect how much you receive from insurance versus the patient and impact your mental health insurance reimbursement.
Common Challenges with BCBS Reimbursement
Many providers face challenges with BCBS reimbursement rates.
Claims may get denied due to missing information or incorrect coding. Payment delays can also happen due to documentation issues.
Another challenge is lack of transparency. Fee schedules are not always publicly available, and providers often need to request them directly.
How to Maximize Your Therapy Reimbursement
If you want to increase your Blue Cross Blue Shield therapy reimbursement, you need a strong billing process.
Start by verifying patient benefits before each session. This helps you understand copays, deductibles, and coverage limits.
Always use correct CPT codes and ensure your documentation supports the service billed.
Submit claims on time and track them regularly to avoid delays.
You can also negotiate better contracts over time as your practice grows.
Many providers also use billing services to improve accuracy and reduce denials.
Real World Example of Therapy Reimbursement
Below is a simple example to help you understand how payment works.
Example Payment Breakdown
Item | Amount |
Therapist Charge | $150 |
Allowed Amount | $120 |
Patient Copay | $30 |
Insurance Payment | $90 |
Total Received | $120 |
This example shows why understanding allowed amounts is essential for revenue planning.
Why Blue Cross Blue Shield Is Important for Therapists
Blue Cross Blue Shield is one of the largest insurance networks in the United States. It covers millions of patients, which makes it a key payer for mental health providers.
Even though reimbursement rates may vary, many providers find it worthwhile due to consistent volume.
You can learn more from the official website of Blue Cross Blue Shield.
Final Thoughts
Blue Cross Blue Shield therapy reimbursement can range widely, but most providers earn between 80 dollars and 160 dollars per session depending on many factors.
Your network status, CPT codes, location, and contract terms all play a role in determining your payment.
By understanding how reimbursement works and improving your billing process, you can increase your revenue and reduce stress in your practice.
FAQ
How much does Blue Cross Blue Shield therapy reimbursement pay per session
Most therapy sessions reimburse between 80 dollars and 160 dollars depending on CPT code, provider type, and location.
Does Blue Cross Blue Shield cover therapy
Yes, most plans cover therapy, but coverage depends on the specific plan, deductible, and whether the provider is in network.
What is the average copay for therapy with BCBS
Copays usually range from 15 dollars to 50 dollars, but some plans may have higher copays depending on coverage.
Do therapists get paid more in network or out of network
In network providers receive lower but steady payments, while out of network providers can charge higher fees but face less predictable reimbursement.
How can I increase my reimbursement
You can increase your Blue Cross Blue Shield therapy reimbursement by using correct CPT codes, submitting clean claims, and verifying patient benefits before sessions.
What is the highest paying CPT code for therapy
CPT code 90837 for a 60 minute session usually pays the highest among standard therapy codes, often between 100 dollars and 160 dollars.
Does location affect BCBS reimbursement rates
Yes, reimbursement rates are higher in cities and states with higher living costs and demand for mental health services.
How long does BCBS take to pay therapy claims
Most claims are paid within 15 to 30 days if submitted correctly, but delays can happen if there are errors or missing information.
Can I negotiate BCBS reimbursement rates
Yes, providers can negotiate rates when signing contracts or renewing agreements, especially if they have strong patient volume.
What happens if I bill more than the allowed amount
If you are in network, you must accept the allowed amount and cannot bill the patient for the difference.
Do all BCBS plans pay the same for therapy
No, payment varies based on the specific plan, employer group, and policy type such as HMO or PPO.
What is coinsurance in therapy billing
Coinsurance is the percentage of the cost that the patient pays after meeting their deductible, usually between 10 percent and 50 percent.
Do therapists need pre authorization for BCBS
Some plans require pre authorization for certain therapy services, especially for long term treatment or specialized care.
Can patients get reimbursed for out of network therapy
Yes, some BCBS plans allow partial reimbursement for out of network therapy, but patients usually need to submit claims themselves.
What is the difference between allowed amount and billed amount
The billed amount is what the provider charges, while the allowed amount is what BCBS agrees to pay based on the contract.
Are telehealth therapy sessions covered by BCBS
Yes, many BCBS plans cover telehealth therapy sessions, and reimbursement rates are often similar to in person visits.




