Hospital billing teams often face confusion when they bill observation care. Many patients stay in a hospital for monitoring but are not admitted as inpatients. In these cases hospitals must follow specific rules for hospital outpatient billing. If the billing team does not follow the correct process, the claim may be denied or underpaid.
Observation care plays an important role in modern healthcare. Physicians use it to monitor patients and decide whether they need admission or can safely go home. Because the patient is not formally admitted, the hospital must treat the encounter as an outpatient service.
This guide explains how to bill outpatient observation services correctly. It also explains key compliance rules, documentation requirements, and common mistakes hospitals should avoid.
Understanding Observation Services in Hospital Settings
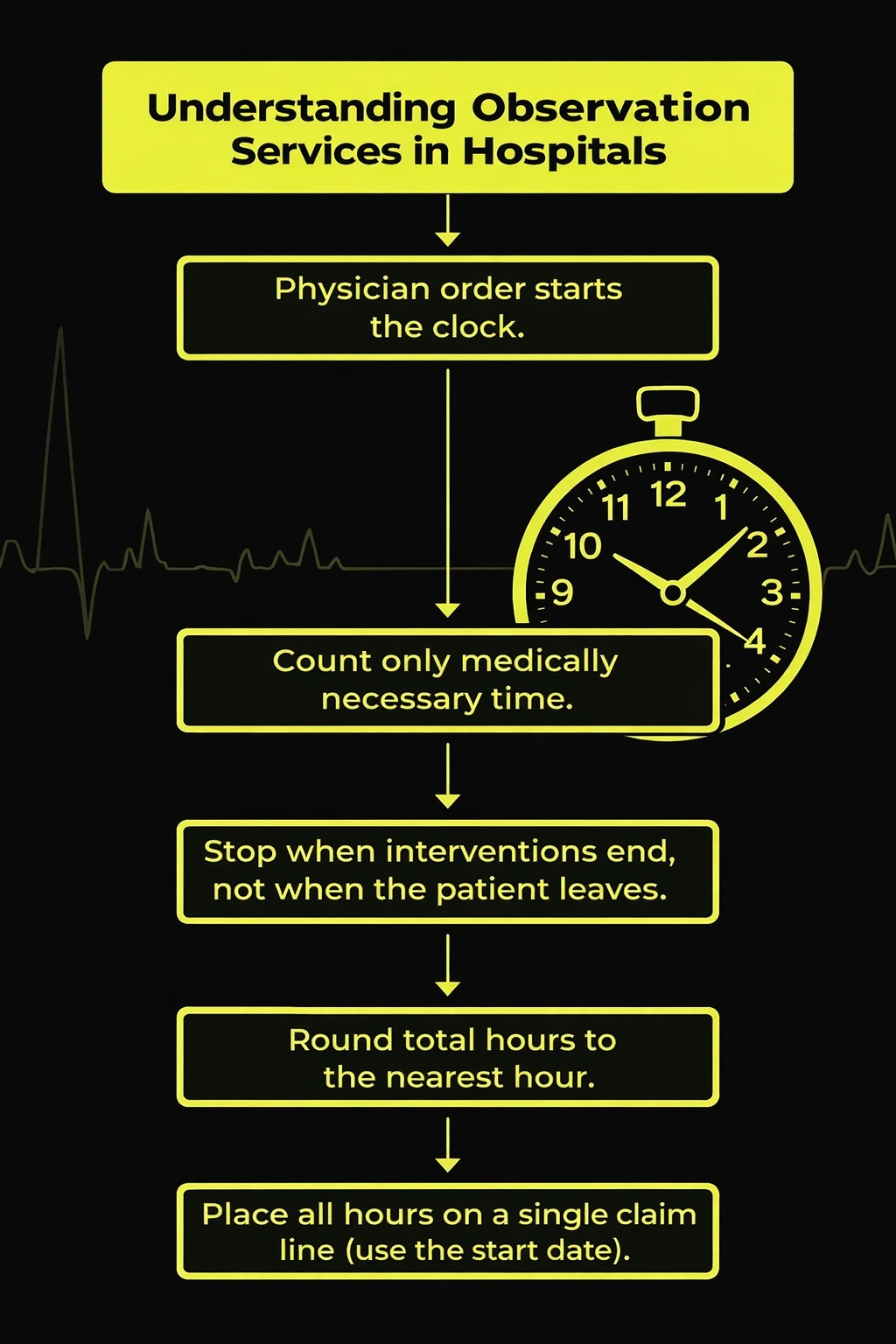
Observation care refers to short term treatment and monitoring provided in a hospital. Doctors order observation services when they need time to evaluate a patient’s condition before deciding on admission or discharge.
These services usually take place after an emergency department visit or outpatient evaluation. During observation, healthcare staff monitor symptoms, review lab results, and provide treatment when needed.
The Centers for Medicare and Medicaid Services defines observation care as ongoing monitoring used to determine whether a patient needs inpatient admission or can be discharged safely.
Observation care often lasts between several hours and one or two days. Hospitals must carefully document the start and end time of observation because billing depends on the total hours provided.
Accurate documentation is essential because payers review the medical record to confirm that observation care was medically necessary.
Why Hospital Outpatient Billing Matters for Observation Services
Observation services fall under outpatient reimbursement rules. Medicare and many commercial payers treat these services differently from inpatient care.
For example, inpatient hospital stays are typically paid under Medicare Part A. Observation services are usually paid under Medicare Part B.
This difference affects how hospitals submit claims and receive reimbursement.
If hospitals incorrectly bill observation services as inpatient care, the claim may fail an audit. On the other hand, if hospitals fail to report observation hours properly, they may receive lower payment.
Correct hospital outpatient billing ensures that hospitals receive appropriate reimbursement and remain compliant with payer rules.
When Observation Services Should Be Used
Observation care is appropriate when a patient needs additional monitoring but does not yet meet inpatient admission criteria.
Doctors may order observation services in several situations. A patient might come to the emergency department with chest pain. The doctor may want to monitor heart activity for several hours before deciding whether admission is necessary.
Another common example involves dehydration or medication reactions. A patient may need IV fluids and monitoring before the physician decides whether discharge is safe.
Observation care can also occur after diagnostic tests or procedures if the physician wants to monitor the patient for complications.
Hospitals must remember that observation care is not meant to replace inpatient admission. It should only be used when the doctor needs short term monitoring before making a clinical decision.
Hospital Outpatient Billing Guidelines for Observation Services
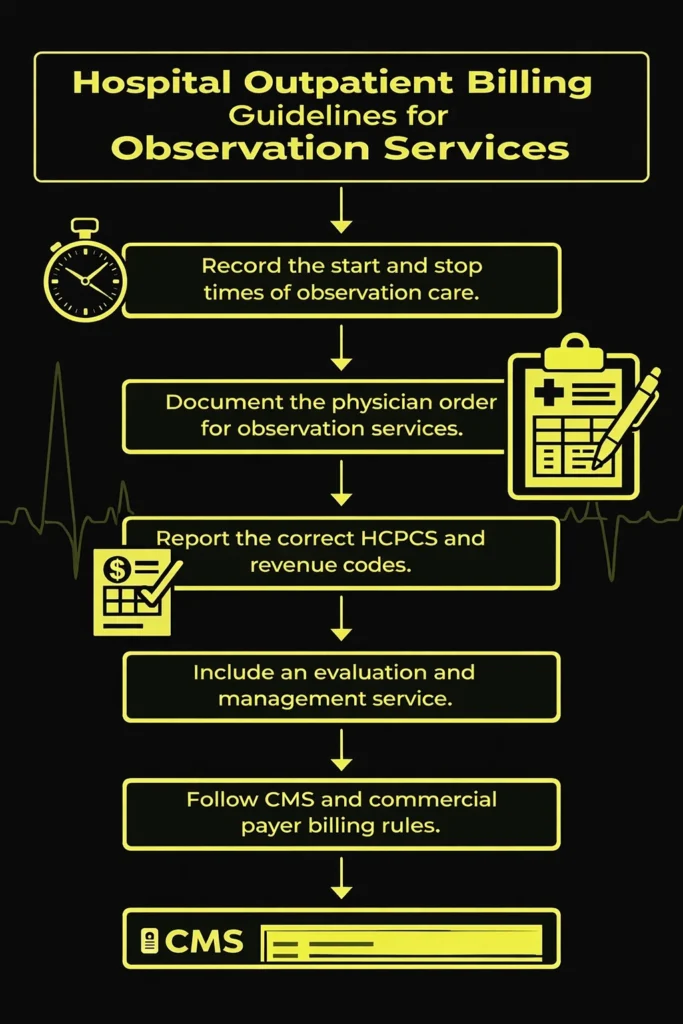
Hospitals must follow clear payer rules when billing observation services. These rules ensure that claims accurately reflect the care provided.
One important guideline involves the start and end time of observation. The observation clock begins when the physician orders observation care and the hospital starts monitoring the patient.
The observation period ends when the patient is discharged or admitted as an inpatient. Time spent waiting for transportation after care ends cannot be included in the billed observation hours.
Hospitals must also document the physician order for observation services. Without a valid physician order, the payer may deny the claim.
Another important rule involves the number of observation hours reported. Hospitals typically report these hours using specific HCPCS codes that track observation time.
Hospitals must also follow hospital outpatient billing guidelines established by CMS and other payers to maintain compliance.
Coding and Claim Submission for Observation Services
Correct coding plays a major role in observation billing.
Hospitals typically report observation services using HCPCS codes such as G0378 for hourly observation care. Each unit represents one hour of observation monitoring.
Another code, G0379, is used when a patient is admitted directly to observation without first visiting the emergency department.
Hospitals also need to include the appropriate revenue codes on the claim form. Many facilities report observation care under revenue code 0762.
In addition to observation codes, the claim must include an evaluation and management service. This visit may occur in the emergency department, clinic, or other outpatient setting.
Correct coding ensures that payers understand the full clinical context of the encounter.
Documentation Requirements for Observation Billing
Proper documentation is one of the most important parts of outpatient billing.
The medical record must clearly show that observation care was medically necessary. It must include a physician order for observation services. The documentation must also include progress notes, nursing records, and the physician’s evaluation.
Medical records should clearly document the patient’s condition and the reason observation care was needed.
Physicians should also record admission notes, daily progress updates, and discharge instructions.
Clear documentation helps protect the hospital during payer audits and supports proper reimbursement.
Need Help Navigating Observation Service Billing?
For example, a patient may initially be admitted as an inpatient but later the hospital determines that inpatient criteria were not met.
Billing Outpatient Services During Inpatient Stay
Sometimes hospitals face situations involving billing outpatient services during inpatient stay.
For example, a patient may initially be admitted as an inpatient but later the hospital determines that inpatient criteria were not met.
In certain cases hospitals may change the status to outpatient observation before discharge. This process requires strict review by the hospital utilization review committee and the attending physician.
Hospitals must document the reason for the status change and inform the patient about the updated classification.
Failure to follow the correct process can create compliance risks and may lead to claim rejections.
Medicare Outpatient Observation Notice Requirements
Hospitals must also inform patients when they receive observation services.
Medicare requires hospitals to give patients a notice called the Medicare Outpatient Observation Notice if they remain in observation status for more than 24 hours.
Hospitals must deliver this notice within 36 hours of the start of observation care.
The notice explains that the patient is receiving outpatient services instead of inpatient care. It also explains how this classification may affect insurance coverage and costs.
Providing this notice is an important compliance requirement for hospitals.
Common Errors in Observation Billing
Observation billing can become complicated when hospitals overlook important rules.
One common mistake involves counting observation hours incorrectly. Some hospitals include time after the patient is medically stable or waiting for discharge.
Another frequent error involves missing physician orders. Without a documented order for observation services, the payer may deny the claim.
Incorrect coding also creates problems. Hospitals sometimes forget to include the required evaluation and management visit on the claim.
Finally, some hospitals fail to provide the required patient notification when observation care extends beyond 24 hours.
Avoiding these errors helps hospitals improve reimbursement accuracy and maintain compliance.
Best Practices for Accurate Hospital Outpatient Billing
Hospitals can improve their observation billing process by following several best practices.
First, they should train physicians and clinical staff on observation criteria and documentation rules.
Second, hospitals should review observation claims before submission to confirm that all codes and documentation are correct.
Third, hospitals should use utilization review teams to confirm that observation care is medically necessary.
Many healthcare organizations also work with experienced billing specialists who understand the complexities of observation billing.
Partnering with experts in Medical Billing Services can help hospitals reduce claim denials and improve financial performance.
Hospitals can also strengthen their billing workflow by using professional Healthcare revenue cycle management services that focus on compliance, coding accuracy, and reimbursement optimization.
These strategies help hospitals manage observation claims more efficiently.
How Technology Helps Improve Observation Billing
Technology plays an important role in modern healthcare billing.
Electronic health record systems allow physicians to place observation orders quickly and record observation hours accurately.
Automated billing software can also track observation time and alert staff when documentation is incomplete.
Advanced analytics tools help hospitals identify billing errors and correct them before claims are submitted.
Hospitals that invest in technology often improve claim accuracy and reduce delays in reimbursement.
The Future of Observation Billing
Observation care continues to grow in modern healthcare systems.
Many hospitals now use observation units to monitor patients who require short term care.
As healthcare regulations evolve, hospitals must remain aware of changes in payer policies and billing guidelines.
Hospitals that maintain strong compliance programs and accurate billing workflows will be better prepared for these changes.
Organizations that understand the details of hospital outpatient billing will continue to improve reimbursement accuracy and financial stability.
For official Medicare policy updates and observation billing guidance, providers can review the CMS website at https://www.cms.gov.
FAQ
What are outpatient observation services in hospitals
Observation services are short term monitoring and treatment provided in a hospital to determine whether a patient needs inpatient admission or can be discharged.
How long can a patient remain in observation status
Observation services usually last less than two days, although the exact duration depends on the patient’s condition and the physician’s decision.
Are observation services considered inpatient care
No. Observation services are classified as outpatient care even if the patient stays in the hospital overnight.
How are observation services billed
Hospitals report observation hours using specific HCPCS codes and include the related evaluation and management services on the claim.
Why is documentation important in observation billing
Documentation proves medical necessity and ensures that the payer understands why observation care was required.
What is the Medicare Outpatient Observation Notice
It is a notice hospitals must give to patients who remain in observation status for more than 24 hours to explain their outpatient classification.
What do we do if the case does not meet the composite rules
If a case does not meet the composite payment rules, the hospital cannot bill the observation service as a composite APC. Instead, the hospital must bill the services separately according to standard hospital outpatient billing rules. In this situation, each service such as the emergency department visit, diagnostic tests, and observation hours will be processed individually. Hospitals must ensure that all required codes and documentation appear correctly on the claim so that payers can review the services accurately.
What does T status mean in outpatient billing
In hospital outpatient billing, T status refers to a payment indicator used in the Medicare Outpatient Prospective Payment System. Services with T status are paid under Ambulatory Payment Classifications and may be subject to multiple procedure discounting. This means when several procedures appear on the same claim, the procedure with the highest payment usually receives full reimbursement while other procedures may receive reduced payment. Understanding T status helps hospitals report procedures correctly and avoid billing errors.
What must be on the claim for a separate observation payment
For a hospital to receive separate payment for observation services, the claim must include several key elements. The claim must show a valid physician order for observation care and the total number of observation hours provided. Hospitals must also report the correct HCPCS code for observation services along with the related evaluation and management visit. In addition, the claim should include the correct revenue codes and supporting documentation. When these elements appear correctly on the claim, payers can process the observation payment accurately.
Error: Contact form not found.