Bill Medicare as a provider can feel complicated at first, but once you understand the process, it becomes manageable and profitable for your practice.
Medicare is a federal health insurance program for people over sixty-five and certain younger people with disabilities. CMS, the Centers for Medicare and Medicaid Services, sets strict rules that every provider must follow.
Knowing these rules, submitting claims accurately, and maintaining compliance are essential to ensure your practice gets paid.
Understanding Medicare and Its Structure
Medicare is divided into four parts, each covering specific types of healthcare services.
For providers, knowing which part covers a service is critical for billing correctly and getting reimbursed on time. Think of each part as a separate bucket that pays for certain types of care.
Part A – Hospital Insurance
Part A covers inpatient hospital care and certain facility-based services. This includes hospital stays, skilled nursing facilities, hospice care, and some home health services if the patient is homebound. Most patients do not pay a monthly premium for Part A if they have paid Medicare taxes through work.
Example: A patient admitted to a hospital after surgery is billed under Part A.
Case Study:
Dr. Johnson treated a patient for pneumonia requiring a hospital stay. The claim was billed to Part A, and Medicare reimbursed the hospital according to inpatient rates.
Key Point: Part A is for hospital and inpatient services, not routine outpatient visits.
Part B – Medical Insurance
Part B covers outpatient care and physician services. This includes office visits, preventive services, lab tests, X-rays, some home health services, and durable medical equipment. Patients pay a monthly premium for Part B.
Example: A preventive wellness visit or outpatient cardiology checkup is billed under Part B.
Case Study:
Dr. Patel initially billed a routine outpatient cardiology checkup under Part A, thinking the hospital setting applied. Medicare denied the claim. After rebilling under Part B, the claim was fully reimbursed.
Key Point: Part B is for office visits, outpatient procedures, and preventive care.
Part C – Medicare Advantage
Part C is a private Medicare plan that provides all Part A and Part B benefits, and often includes Part D for drugs. Medicare Advantage plans are offered by private insurance companies approved by Medicare.
Example: A patient enrolled in a Medicare Advantage plan visits your clinic for an outpatient procedure. Even though this is technically a Part B service, you bill the Medicare Advantage plan (Part C) instead of Original Medicare.
Case Study:
A primary care clinic saw a patient with a Medicare Advantage plan requiring prior authorization for imaging. By verifying coverage in advance, the clinic avoided a denied claim and received payment promptly.
Key Point: Part C is billed through the Medicare Advantage plan, and rules may differ from Original Medicare. Always check eligibility and pre-authorization requirements.
Part D – Prescription Drug Coverage
Part D covers prescription medications. Patients enroll in these plans separately and pay a monthly premium. Providers prescribe medications, but billing for the drugs is handled by pharmacies and insurance.
Example: A patient recovering from surgery is prescribed heart medications. Coverage comes from Part D.
Key Point: Part D covers drugs only, and providers’ role is primarily prescribing and documenting the medication.
Quick Reference Table: Medicare Parts for Providers
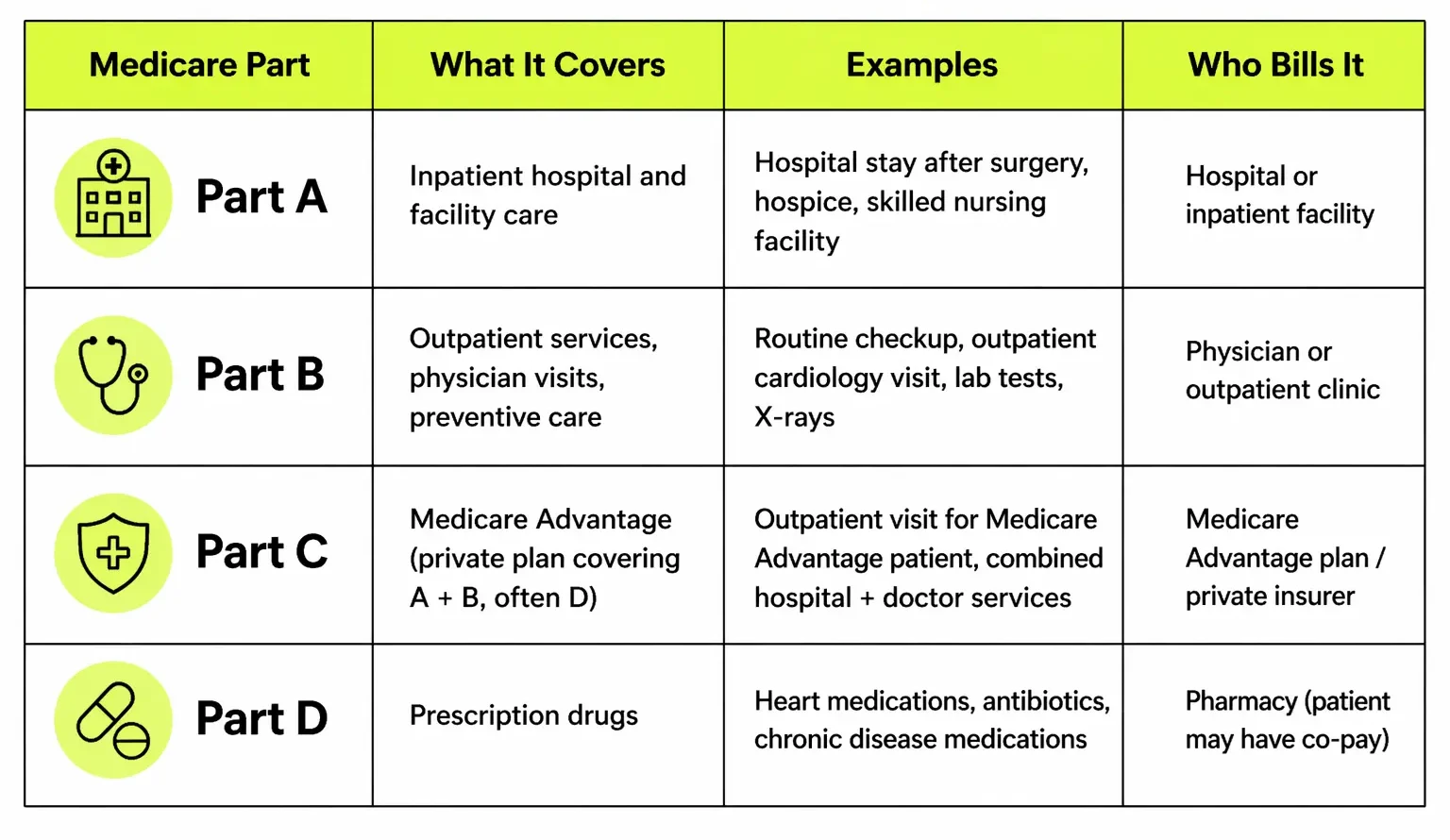
The Medicare Billing Process
Billing begins the moment you see a patient. Collect complete patient information, including Medicare number, eligibility, and coverage type.
Eligibility verification is important because Medicare will not pay for services for patients who are not covered.
Document every service carefully. Include:
- Diagnosis
- Procedure performed
- Date of service
- Medical necessity
Accurate documentation protects your practice from audits and ensures claims are supported with evidence.
Claims are submitted using forms like CMS-1500 for professional services or UB-04 for institutional services.
Electronic submission is faster and reduces errors. Many billing software systems integrate directly with Medicare’s electronic system, making the process smoother.
Once a claim is submitted, Medicare reviews it based on coding, documentation, and eligibility.
If everything is correct, payment is issued. If there are errors, the claim is denied and must be corrected and resubmitted.

Common Challenges in Medicare Billing
Even experienced providers face challenges. Coding errors are one of the most common. Each service requires a CPT or HCPCS code. Using the wrong code or missing a modifier can result in denied claims.
Documentation is another challenge. Medicare auditors may request patient records to verify claims. Incomplete notes or missing justification can trigger audits or repayment demands.
Eligibility verification is essential. Some patients may have Medicare Advantage plans that require pre-authorization for certain services. Failing to check eligibility can result in denied claims.
Case Study:
A dermatology clinic repeatedly submitted claims for advanced skin treatments without checking patient eligibility. The claims were denied because the services required prior authorization under the patient’s Medicare Advantage plan. After implementing a verification protocol, denials dropped by 70%, improving revenue.
Tips for Accurate Medicare Billing
- Verify Eligibility: Confirm patient coverage before providing services using Medicare’s eligibility verification system or by calling Medicare directly.
- Document Thoroughly: Include diagnosis codes, procedures, and medical necessity. Complete documentation prevents denials and protects your practice in audits.
- Submit Electronically: Electronic claims are processed faster, reduce errors, and allow real-time tracking.
- Understand Modifiers: Some services require specific modifiers to indicate unusual circumstances. Incorrect coding is a leading cause of denials.
- Follow Up on Claims: Monitor unpaid claims regularly. Payment delays may occur due to missing documentation or processing errors.

CMS Guidelines and Compliance
CMS guidelines cover enrollment, documentation, coding, claims, and reporting. Noncompliance can result in fines, repayment, or exclusion from Medicare.
CMS provides manuals, webinars, and updates to help providers stay compliant. Regularly reviewing these resources prevents claim denials and speeds reimbursement.
Case Study:
A primary care clinic failed to apply the correct preventive care code for annual wellness visits. An audit revealed this issue. After reviewing CMS guidelines, the clinic corrected its coding protocol and avoided future penalties.
Outsourcing Medical Billing
Outsourcing billing saves time, reduces errors, and improves cash flow. Professional billing services handle coding, claim submission, and follow-up, allowing providers to focus on patient care.
Choose a reputable company experienced in Medicare billing. Verify compliance with CMS guidelines and ensure transparent reporting. The investment often pays off with fewer denials and faster revenue.
Example:
A small pediatric practice outsourced Medicare billing and reduced claim denials from 15% to 4% within six months. Staff were freed up to spend more time with patients, increasing patient satisfaction.
Staying Up to Date with Medicare
Medicare rules change frequently. Staying informed is essential for accurate billing. Subscribe to CMS updates, attend webinars, and review annual CPT and HCPCS changes. Educate staff and update billing processes to maintain compliance.

Common Mistakes Providers Make
- Incorrect coding: Using outdated or wrong codes delays payment or triggers audits.
- Failing to verify eligibility: Denied claims waste time and revenue.
- Incomplete documentation: Missing details can result in rejected claims.
- Ignoring denied claims: Not appealing claims can cost thousands in lost revenue.
Case Study:
A chiropractic office ignored denied claims for several weeks. After hiring a part-time billing coordinator, they recovered $18,000 in previously denied claims within three months.
How to Appeal Denied Claims
Medicare has a structured appeals process. Review the denial reason, correct errors, add missing documentation, and resubmit with explanation. Appeals include:
- Reconsideration
- Administrative law judge review
- Medicare Appeals Council review
Prompt action ensures faster recovery of lost payments.

Resources for Providers
CMS provides manuals, billing guides, coding resources, and enrollment instructions. Professional organizations like the American Medical Association or Medical Group Management Association offer additional guidance.
Real-World Example of a Successful Billing Workflow
A mid-sized internal medicine practice implemented the following workflow:
- Verify eligibility at scheduling.
- Document services in EMR with correct diagnosis and procedure codes.
- Submit claims electronically daily.
- Track all pending claims weekly.
- Audit documentation quarterly.
Within six months, claim denials decreased by 60%, average reimbursement time dropped from 35 days to 18 days, and staff efficiency increased.
Key Takeaways
Billing Medicare as a provider requires precision, documentation, and compliance. By understanding the Medicare billing process, verifying eligibility, coding correctly, submitting claims electronically, and following up on unpaid claims, your practice can receive timely reimbursement. Staying informed about CMS rules and coding updates protects your practice and maximizes revenue.
Need Help Navigating Medicare Billing as a Provider?
Get practical guidance to maximize reimbursements and stay compliant.
FAQ
How long does it take to get paid by Medicare?
Payment typically takes 14 to 30 days for electronic claims if documentation is correct and submission is accurate.
Do I need to be enrolled in Medicare to bill it?
Yes, providers must enroll and have a Medicare provider number before submitting claims.
Can I appeal a denied Medicare claim?
Yes, Medicare has a multi-level appeals process. Timely submission with proper documentation is essential.
What is the difference between Part A and Part B billing?
Part A covers inpatient and hospital services. Part B covers outpatient services, physician visits, and preventive care.
Are electronic claims required for Medicare?
Electronic claims are preferred for faster processing, but paper claims are still accepted in some cases.
What is a common mistake providers make when billing Medicare?
Incorrect coding, failing to verify eligibility, and incomplete documentation are the most common mistakes.