If you want to build a strong and stable healthcare practice, you must understand CMS Credentialing Requirements from the very beginning. This process is not just a formality. It is one of the most important steps that decides whether you can work with Medicare and receive payments without problems.
Many providers underestimate how important this process is. They often rush through applications or miss small details. These small mistakes can lead to major delays, rejected claims, and lost revenue. That is why taking time to understand CMS Credentialing Requirements can make a big difference in your success.
Credentialing is a process where your qualifications, experience, and professional background are reviewed. CMS wants to make sure that every provider meets strict standards before they are allowed to treat patients under Medicare. This helps protect patients and keeps the healthcare system reliable.
When you follow CMS Credentialing Requirements correctly, you build trust, avoid stress, and create a smooth billing system. This guide will help you understand every part of the process in simple language so you can move forward with confidence.
What Are CMS Credentialing Requirements
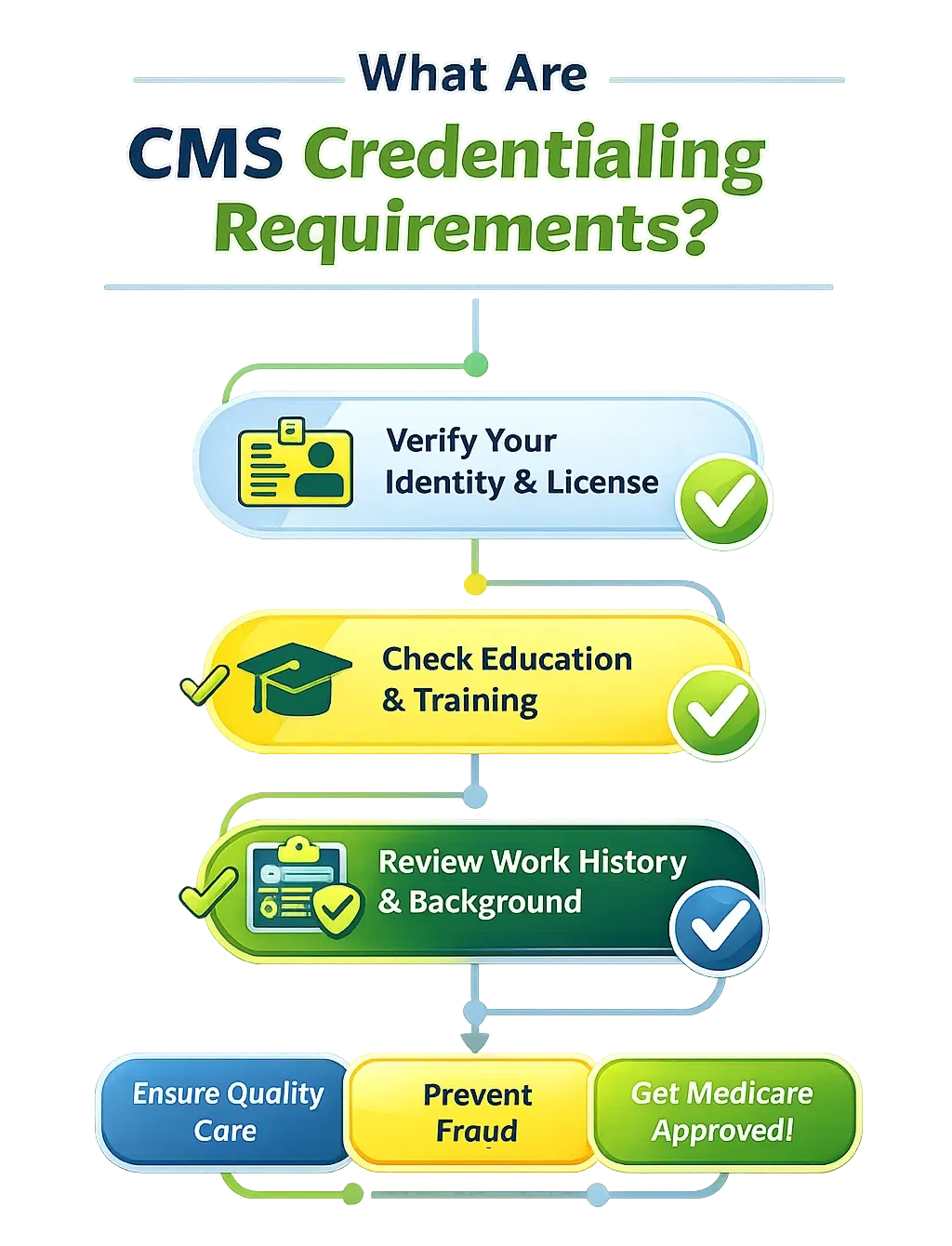
CMS Credentialing Requirements are rules created by the Centers for Medicare and Medicaid Services. These rules help verify that healthcare providers are qualified and safe to deliver care.
The process checks your identity, your license, your education, and your work history. CMS reviews everything carefully to make sure that you meet their standards. They also check for any past issues that may affect your approval.
This process is important because it ensures that only trained and licensed providers work with Medicare patients. It also helps prevent fraud and protects patient safety.
When you complete CMS Credentialing Requirements, you prove that you are a trusted provider who meets national healthcare standards.
Why CMS Credentialing Requirements Matter
Understanding CMS Credentialing Requirements is important because it directly affects your income and your ability to serve patients.
Without credentialing, you cannot bill Medicare. This means you cannot receive payments for services provided to Medicare patients. For many providers, this can limit growth and reduce opportunities.
Credentialing also helps build your professional image. Patients feel more comfortable choosing a provider who is approved by Medicare. It shows that you meet high standards and follow proper rules.
Another important reason is compliance. Healthcare laws are strict, and mistakes can lead to penalties. Following CMS enrollment guidelines helps you stay compliant and avoid legal issues.
In simple terms, credentialing is not just a requirement. It is a key part of running a successful healthcare practice.
Who Needs CMS Credentialing
CMS Credentialing Requirements apply to many types of healthcare providers.
Doctors, nurses, therapists, and specialists must complete the process if they want to work with Medicare patients. Each provider must be verified individually.
Group practices also need credentialing. Every provider in the group must complete healthcare provider credentialing, and the organization must enroll as well.
Hospitals, clinics, laboratories, and medical suppliers must also follow these rules. This ensures that every part of patient care meets CMS standards.
If you plan to work in the healthcare field and serve Medicare patients, credentialing is not optional. It is required.
Understanding the Provider Enrollment Process
The provider enrollment process is the main way to complete CMS Credentialing Requirements. It may seem complex, but it becomes easier when you understand each step.
The first step is preparation. You need to collect all your documents before starting your application. This includes your license, education certificates, work history, and tax details.
The next step is creating an account in the PECOS system. This is the official online platform used by CMS for enrollment.
After creating your account, you submit your application. You must provide accurate and complete information.
Once your application is submitted, CMS reviews it carefully. They may ask for additional information if something is missing or unclear.
Finally, after approval, you receive your Medicare billing privileges. This allows you to start seeing patients and submitting claims.
The provider enrollment process requires patience and attention to detail, but it is manageable when done correctly.
Key Documents Required for Credentialing

To meet CMS Credentialing Requirements, you must provide several important documents.
Your professional license is one of the most important documents. It must be active and valid in your state.
You also need proof of education. This includes your degree and any certifications related to your field.
Training records are required as well. These show that you have completed necessary programs and have the skills needed to provide care.
Work history is another key requirement. CMS reviews your past experience and checks for any gaps.
You must also provide identification and tax information. This ensures that payments are processed correctly and sent to the right place.
Keeping your documents organized and updated can make the process much easier.
Common Mistakes in CMS Credentialing
Many providers face delays because of simple mistakes.
One common mistake is submitting incomplete applications. Missing details can slow down the process or lead to rejection.
Another issue is providing outdated information. Expired licenses or incorrect details can create problems during review.
Some providers also fail to respond to CMS requests on time. This can delay approval and affect your ability to start billing.
To avoid these issues, always review your application carefully. Make sure everything is complete and accurate before submission.
How Long Does Credentialing Take
The time required to complete CMS Credentialing Requirements can vary.
In most cases, the process takes a few weeks to a few months. If your application is accurate and complete, it may move faster.
Delays usually happen when CMS needs additional information or finds errors.
You can reduce delays by double checking your application and responding quickly to any requests.
Being patient and prepared is the best way to handle this process.
Revalidation and Ongoing Compliance
Credentialing is not a one time task. Providers must continue to meet CMS Credentialing Requirements even after approval.
CMS requires providers to revalidate their information regularly. This ensures that all records remain accurate.
If you fail to revalidate, your billing privileges may be suspended. This can lead to payment delays and loss of revenue.
Following CMS enrollment guidelines helps you stay compliant and avoid problems.
Keeping your information updated is an important part of long term success.
Benefits of Medicare Credentialing
Medicare credentialing offers many benefits for providers.
It allows you to serve a large and growing patient base. This can help you expand your practice and increase your income.
It also builds trust with patients. When they know you are approved by Medicare, they feel more confident in your care.
Credentialing also helps ensure smooth billing. Providers who follow CMS Credentialing Requirements face fewer claim issues and receive payments more reliably.
In the long run, credentialing supports both growth and stability.
Challenges Providers Face
Many providers find CMS Credentialing Requirements difficult to manage at first.
The process can feel overwhelming because it involves many steps and documents.
Rules may change over time, which makes it harder to stay updated.
Providers who work in multiple locations may need separate enrollments, which increases the workload.
Despite these challenges, proper planning and organization can make the process much easier.
Importance of Accurate Information
Accuracy is one of the most important parts of CMS Credentialing Requirements.
Even small errors can lead to delays or rejection. Incorrect information can also affect your payments.
Always review your application carefully. Make sure every detail is correct before submitting it.
Keeping your records updated can help you avoid problems in the future.
How Technology Helps in Credentialing
Technology has made credentialing much easier for providers.
The PECOS system allows you to submit applications online. This reduces paperwork and saves time.
Digital tools can help you organize your documents and track your application status.
These tools reduce errors and make the process more efficient.
Using technology wisely can improve your overall experience with credentialing.
Confused About CMS Credentialing Requirements?
Learn how to complete your enrollment, avoid delays, and get approved without stress.
Tips for a Smooth Credentialing Process
To meet CMS Credentialing Requirements successfully, you need to stay organized and focused.
- Start by gathering all your documents before beginning the process.
- Make sure your information is accurate and up to date.
- Submit your application through PECOS and track its progress regularly.
- Respond quickly to any requests from CMS to avoid delays.
- If needed, you can seek professional help to guide you through the process.
Future of CMS Credentialing
The healthcare industry continues to evolve, and CMS Credentialing Requirements are changing as well.
There is a growing focus on digital systems and faster approvals. This will make the process easier in the future.
However, the need for accuracy and compliance will always remain. Providers must stay informed and prepared.
For official updates and detailed information, visit the CMS website https://www.cms.gov
Key Takeaways
CMS Credentialing Requirements are a key part of working with Medicare. They ensure quality care, build trust, and support smooth billing.
By understanding the process and following each step carefully, you can avoid delays and grow your practice with confidence.
Stay organized, provide accurate information, and keep your records updated. With the right approach, credentialing becomes simple and manageable.
FAQ
What are CMS Credentialing Requirements
CMS Credentialing Requirements are rules that providers must follow to enroll in Medicare and receive payments.
How long does credentialing take
The process usually takes a few weeks to a few months depending on your application.
Why is medicare credentialing important
It allows providers to treat Medicare patients and receive payments without delays.
Can I complete credentialing myself
Yes, but many providers choose expert help to avoid mistakes.
What happens if I do not revalidate
You may lose your billing privileges and face payment issues.
What is the difference between credentialing and enrollment
Credentialing is the process of verifying your qualifications, while enrollment is submitting your details to CMS so you can start billing Medicare. Both are part of CMS Credentialing Requirements.
Do I need credentialing for each practice location
Yes, if you work in multiple locations, you may need to enroll each location separately depending on how your practice is set up.
Can credentialing be denied
Yes, CMS can deny your application if your information is incomplete, incorrect, or if there are issues with your license or background.
How often do I need to update my CMS information
You must update your information whenever there are changes and complete revalidation when CMS requests it.
What is PECOS and why is it important
PECOS is the online system used by CMS to manage enrollment. It allows you to submit and track your credentialing application easily.
Can I bill Medicare while my credentialing is in process
In most cases, you must wait until your application is approved before billing Medicare.
What happens if my credentialing expires
If your credentialing is not updated or revalidated, your billing privileges may be stopped, which can affect your payments.