Running a clinic takes a lot of time, care, and attention. Your team has to manage patients, appointments, records, insurance details, and payments every day. When billing problems happen, they can slow down your revenue and create extra stress for your staff.
Many clinic billing problems start with small mistakes. A wrong code, missing patient detail, skipped insurance check, or delayed follow-up can lead to claim denials and late payments.
Why Clinic Billing Problems Matter
Billing is not just paperwork. It directly affects your clinic’s cash flow, staff workload, and patient experience. When claims do not get paid on time, clinics may struggle with revenue gaps, more phone calls, and extra admin work.
A smooth billing process helps clinics get paid faster, reduce errors, and keep more focus on patient care.
What This Infographic Covers
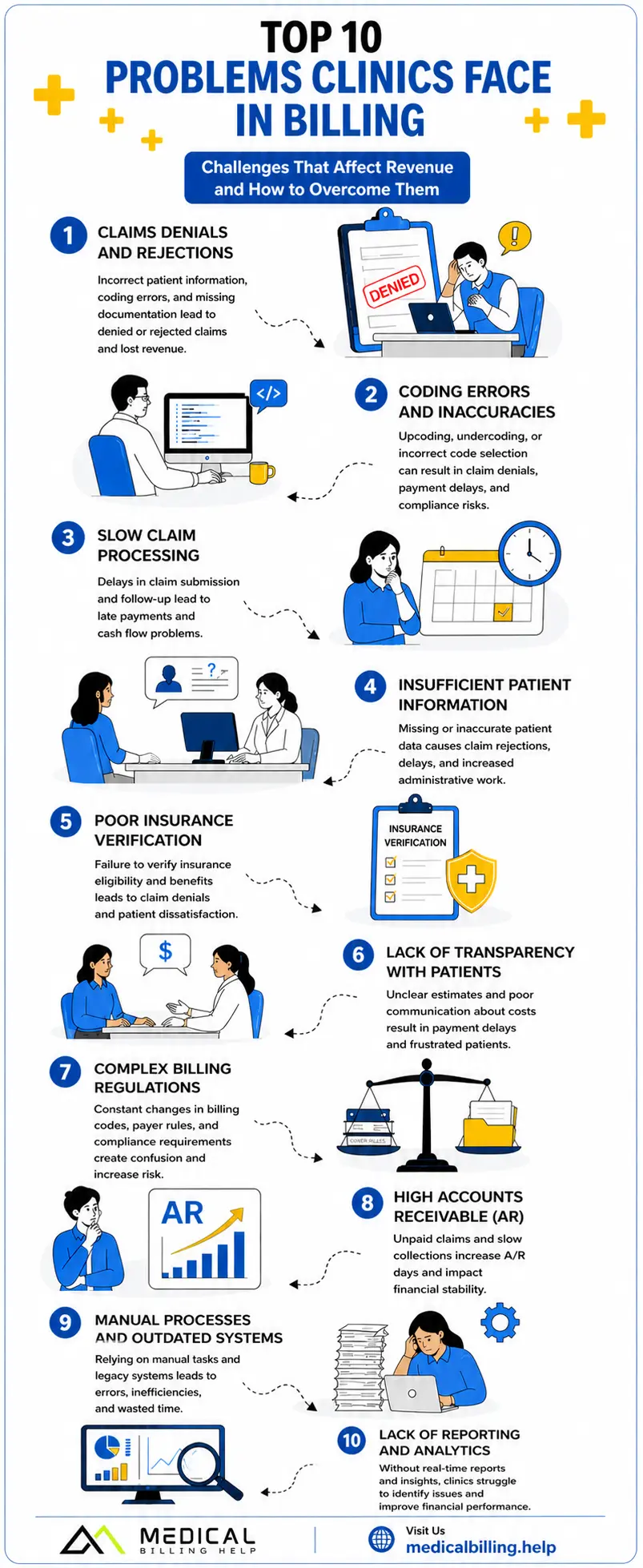
This infographic explains the top 10 problems clinics face in billing, including claim denials, coding errors, insurance verification issues, slow claim processing, and high accounts receivable.
Use it as a quick guide to understand where billing problems usually happen and what your clinic can do to avoid them.
10 Common Clinic Billing Problems
Need help fixing Clinic Billing Problems?
Get expert billing support today and keep your clinic focused on patient care.
FAQs
What are the most common clinic billing problems?
The most common clinic billing problems include claim denials, coding errors, missing patient details, insurance verification issues, slow follow-ups, and high accounts receivable.
Why do clinics face medical billing problems?
Clinics face medical billing problems because billing rules change often. Staff may also miss details, use wrong codes, or face delays from insurance companies.
What causes claim denials in medical billing?
Claim denials usually happen due to incorrect coding, missing information, expired insurance, or late claim submission.
How can clinics reduce claim denials?
Clinics can reduce claim denials by verifying insurance, checking patient details, using correct codes, and submitting clean claims on time.
Why is insurance verification important in clinic billing?
Insurance verification confirms patient coverage before treatment. It helps avoid denied claims and reduces billing delays.
What are coding errors in medical billing?
Coding errors happen when wrong medical codes are used. This can lead to claim rejections, delays, or lower payments.
What is accounts receivable (AR) in medical billing?
Accounts receivable (AR) is the money clinics are waiting to collect from insurance companies or patients after services are provided.
How can clinics reduce accounts receivable days?
Clinics can reduce AR days by submitting accurate claims, following up regularly, and resolving denied claims quickly.
What causes delays in medical billing payments?
Delays happen due to claim errors, missing documents, slow insurance response, or lack of proper follow-up.
What is denial management in medical billing?
Denial management is the process of reviewing denied claims, fixing errors, and resubmitting them to get paid.
How can clinics improve their billing process?
Clinics can improve billing by training staff, using updated systems, checking data carefully, and following up on claims.
Should clinics outsource medical billing?
Yes, many clinics outsource medical billing to reduce errors, save time, and improve cash flow with expert support.
How can MedicalBilling.Help support clinics?
MedicalBilling.Help supports clinics by handling daily billing tasks such as claim submission, insurance verification, coding support, denial management, payment posting, and AR follow-up. This helps clinics reduce billing errors, get paid faster, and spend more time on patient care.




