MRI CPT Codes help medical billing teams report MRI scans the right way. MRI stands for magnetic resonance imaging. Doctors use MRI scans to see the brain, spine, joints, abdomen, pelvis, breast, heart, and blood vessels. These scans help doctors find injuries, tumors, nerve issues, swelling, pain causes, and many other health problems.
MRI claims often need careful billing because they cost more than many basic imaging services. Payers may check the body area, diagnosis, contrast use, prior approval, and provider notes before they pay the claim. A small coding mistake can lead to a denial, delay, or request for medical records.
CPT codes are five digit codes that describe medical services and procedures. The American Medical Association says CPT codes give healthcare teams a common way to report care, tests, and procedures. You can learn more from the official American Medical Association CPT page.
This guide explains commonly used MRI CPT Codes in simple words. It gives clear tables for common MRI exams and also explains how billers can avoid common claim mistakes.
MRI billing codes
MRI billing starts with the final report. The coder should not choose a code from the schedule alone. The final report should show the body area, contrast use, exam name, findings, and reason for the scan.
The most important detail is the body part. A brain MRI uses different codes than a spine MRI. A lumbar spine MRI uses different codes than a cervical spine MRI. A knee MRI also uses different codes than a non joint leg MRI.
The next important detail is contrast. Some MRI exams happen without contrast. Some happen with contrast. Some happen first without contrast and then again with contrast. Many MRI CPT Codes change based on that detail.
A clean claim should match the order, final report, diagnosis, and payer approval. If the payer approved a scan without contrast but the claim shows a scan with and without contrast, the payer may deny the claim. The billing team should check this before sending the claim.
MRI procedure codes
The table below explains common MRI CPT Codes for the brain, orbit, face, neck, and spine. These codes appear often in neurology, pain care, injury care, cancer care, and emergency care.
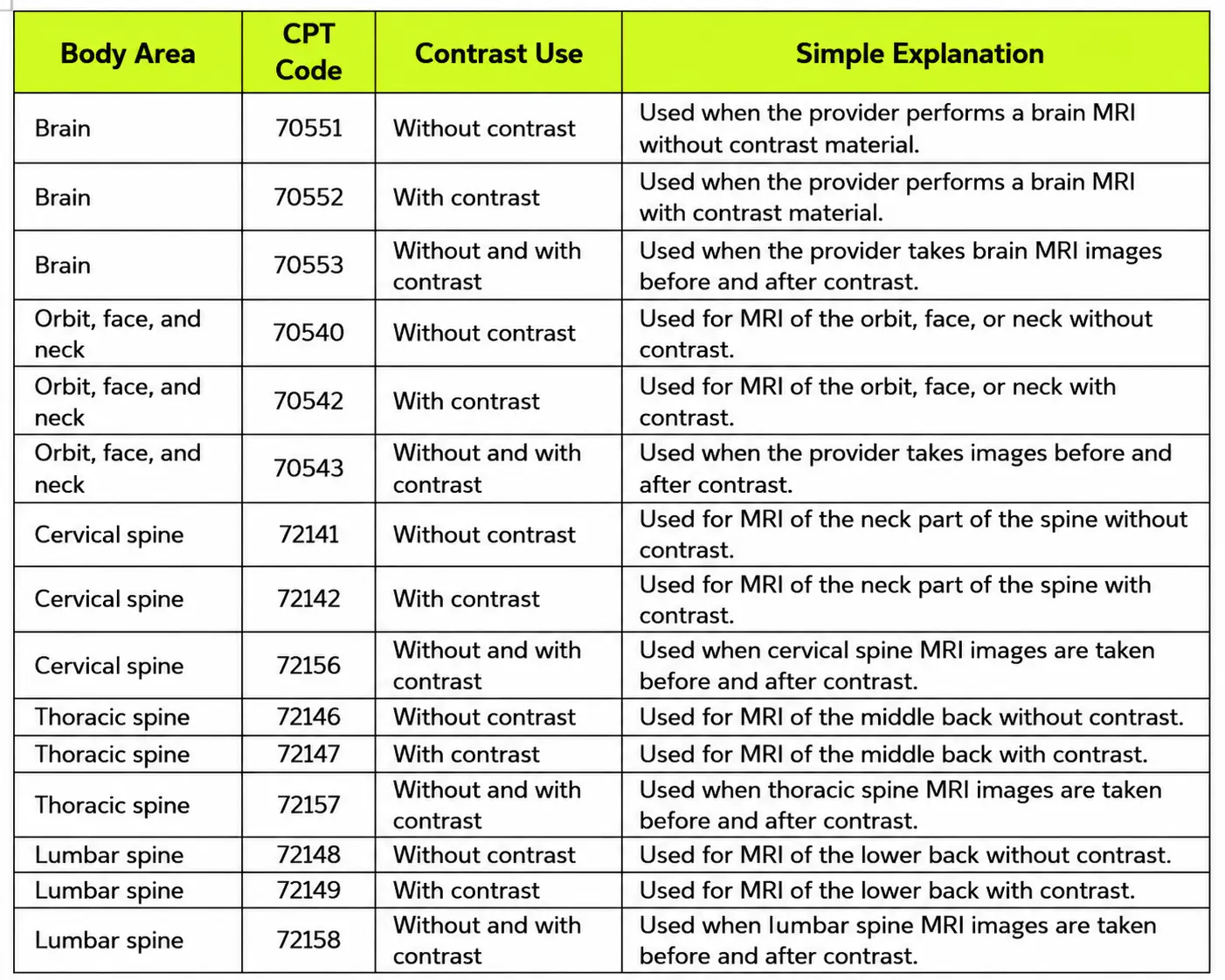
Brain MRI claims often support care for headaches, seizures, memory issues, dizziness, stroke symptoms, tumors, or multiple sclerosis. The report should clearly show whether the provider used contrast.
Spine MRI claims often support care for neck pain, back pain, numbness, tingling, nerve pain, disc disease, trauma, or surgery follow up. The coder must choose the code for the exact spine area. A cervical spine MRI is not the same as a lumbar spine MRI.
If the provider scans more than one spine area, the documentation must support each area. The billing team should also check payer rules because some payers review multiple MRI services on the same date.
Common Joint and Extremity MRI CPT Codes
Joint and extremity MRI services appear often in orthopedic care, sports medicine, podiatry, pain care, and injury care. A joint MRI focuses on a joint, such as the shoulder, elbow, wrist, hip, knee, ankle, or foot. A non joint MRI focuses on soft tissue outside a joint.
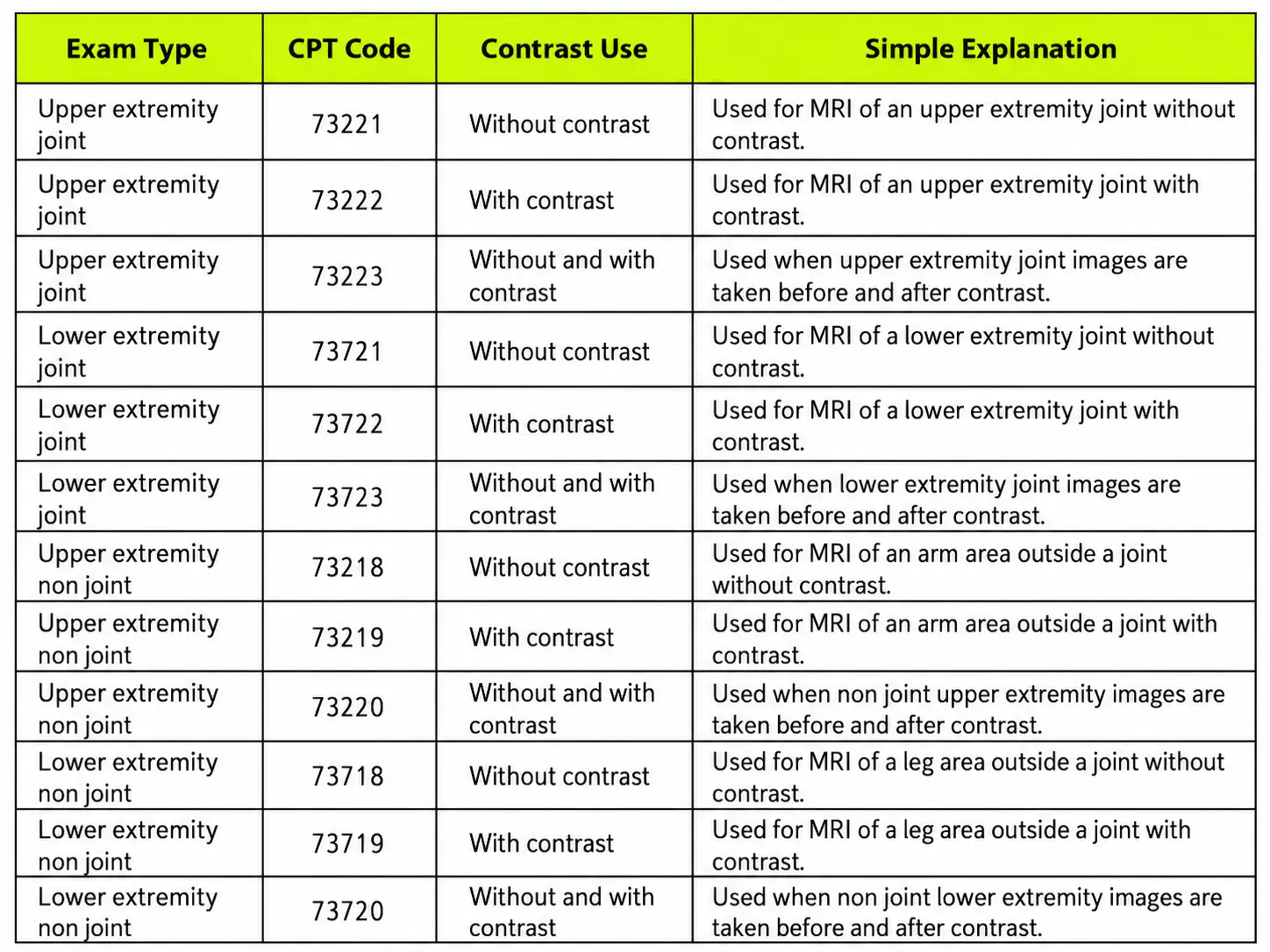
The report must show the exact body area. For example, a knee MRI usually uses a lower extremity joint code. A thigh soft tissue MRI usually uses a lower extremity non joint code. These details matter because the payer reviews the code against the medical record.
The coder should also check whether the report supports contrast. Many routine joint MRI exams happen without contrast. Some exams need contrast when the doctor wants more detail or when the patient has a special clinical need. The report should support the code billed.
MRI scan CPT code
The table below covers common MRI CPT Codes for the chest, abdomen, pelvis, breast, and heart. These services often need strong notes because payers may review the reason for the scan.
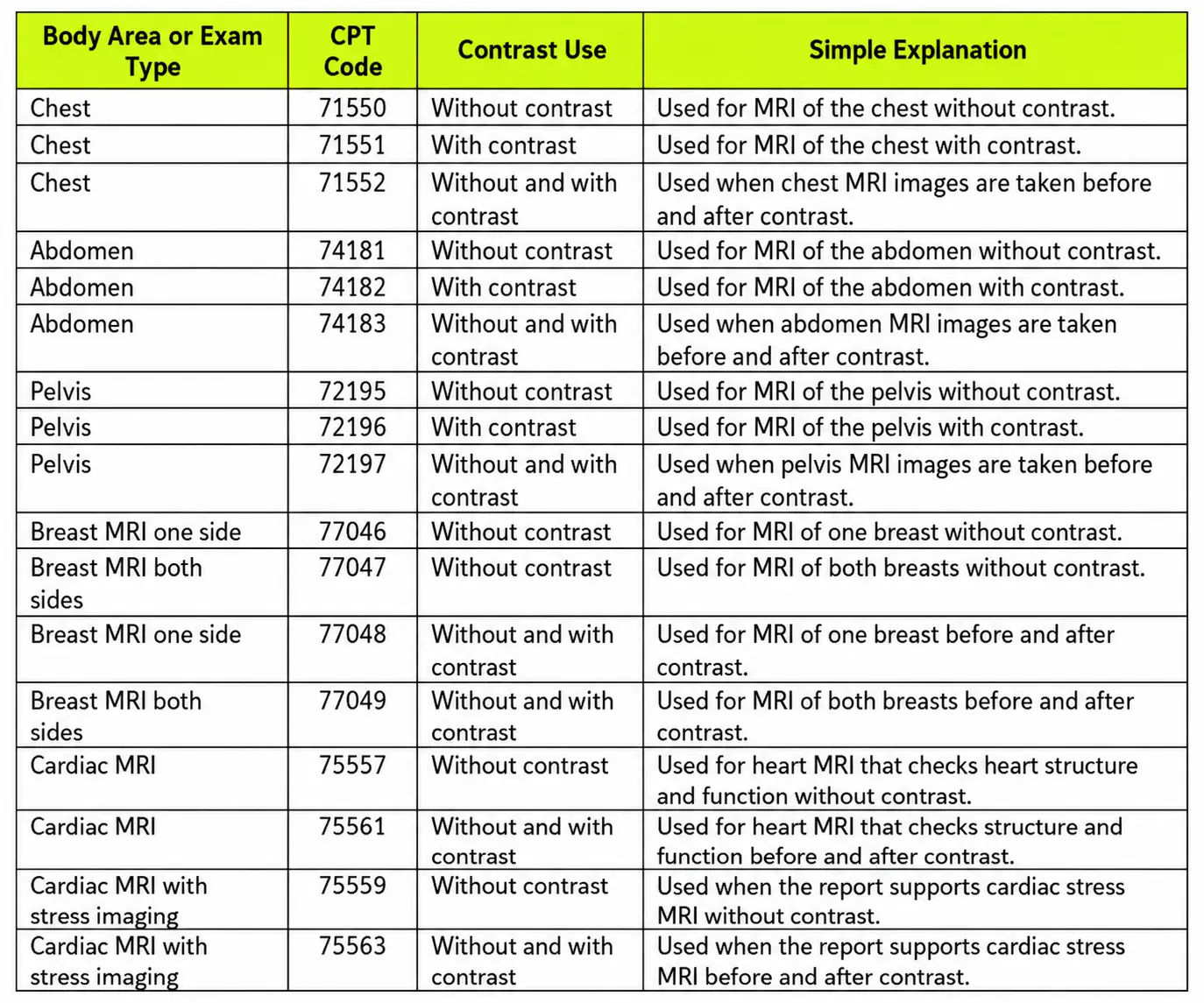
Abdomen MRI claims may support liver, kidney, pancreas, adrenal, or bile duct concerns. Pelvis MRI claims may support pelvic pain, prostate care, fistula checks, rectal cancer staging, or gynecologic concerns.
Breast MRI has its own code set. Coders should not use chest MRI codes when the report clearly describes breast MRI. The report should show whether the exam looked at one breast or both breasts. It should also show whether the provider used contrast.
Cardiac MRI focuses on the heart. These claims can need prior approval and clear diagnosis support. The billing team should review payer rules before the scan when possible.
Common MRA CPT Codes
MRA means magnetic resonance angiography. It looks at blood vessels. MRA codes are different from standard MRI codes. The coder should report an MRA code when the report describes a vessel study.
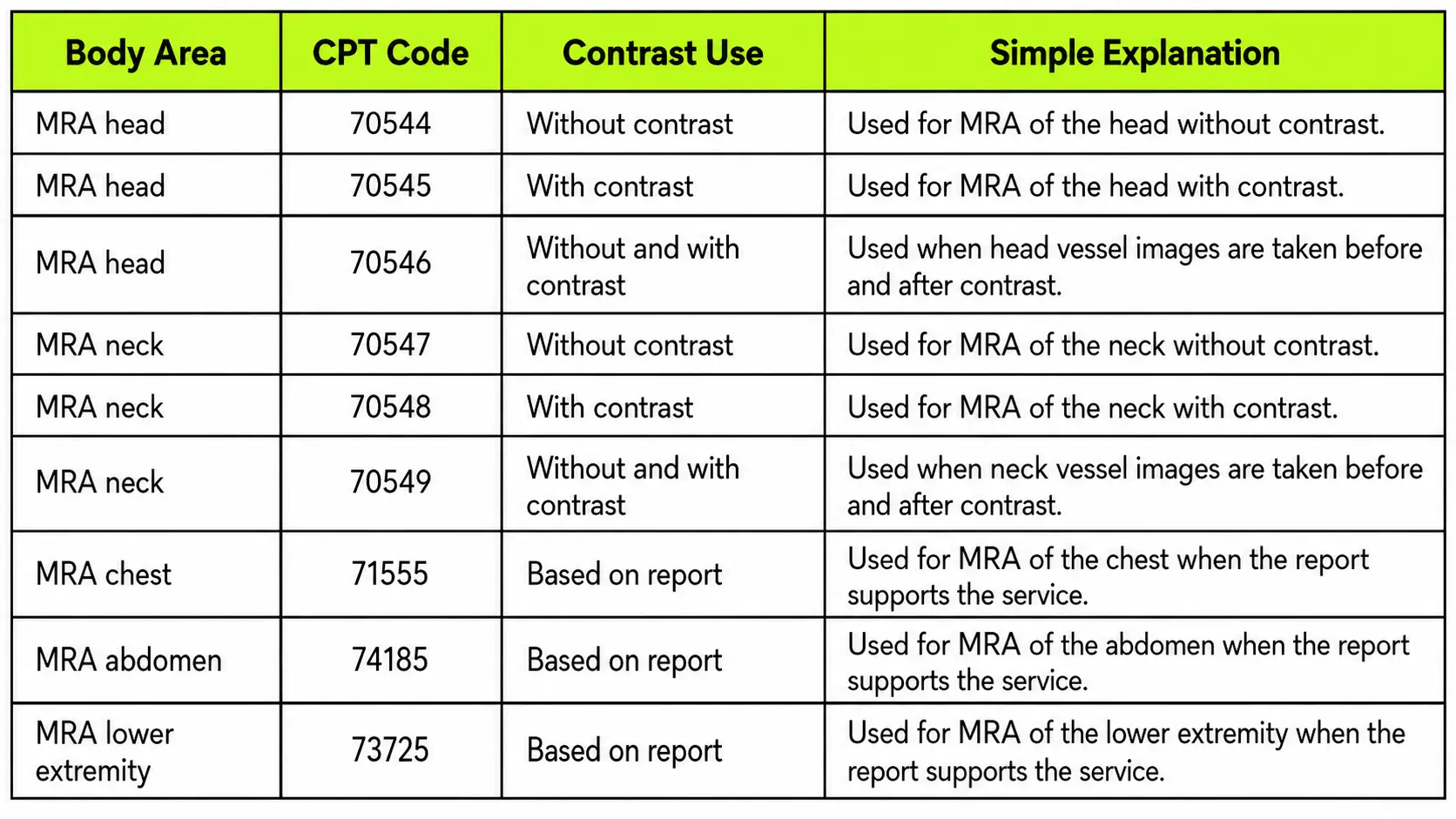
MRA may support care for aneurysm, narrowing of blood vessels, clot concern, blood flow problems, or vascular malformation. The report should name the vessel area and show why the study was needed.
A common billing mistake happens when staff bill MRA as MRI or MRI as MRA. These services sound close, but they do not describe the same exam. The final report should guide the code.
Radiology CPT Codes
MRI coding sits inside the larger imaging code set. These codes help payers understand what imaging service the provider performed. A clean imaging claim should match the order, report, diagnosis, prior approval, provider details, and place of service.
For MRI claims, the final report matters most. It should include the exam title, body area, contrast use, technique, findings, and impression. The coder should review all of these details before claim submission.
The diagnosis also matters. A payer may deny an MRI claim when the diagnosis does not support the scan. For example, a general pain diagnosis may not support some MRI services unless the medical record shows more detail. The provider note may need to show symptom length, failed treatment, injury history, nerve signs, cancer concern, or follow up reason.
How Contrast Changes MRI CPT Codes
Contrast can change the code. That is why coders must read the contrast section of the report. Without contrast means the provider did not give contrast material. With contrast means the provider gave contrast and performed the scan with contrast images. Without and with contrast means the provider took images before contrast and again after contrast.
A claim should not report without and with contrast unless the report supports both parts. If the order asked for contrast but the patient did not receive contrast, the coder should not bill a contrast code. The performed service must guide the claim.
Payers may also check whether the diagnosis supports contrast. Some conditions need contrast because the doctor needs more detail. Other cases may not support it. The provider should document why contrast helped answer the clinical question.
Prior Authorization for MRI Claims
Many payers require prior authorization before MRI services. The front desk or authorization team should check the payer rule before the scan date. A claim can deny even when the code is correct if the payer required approval and the office did not get it.
The approval should match the body area and contrast use. If the payer approved MRI brain without contrast, but the provider performed MRI brain without and with contrast, the team may need to update the approval before billing.
The approval should also match the place of service and valid date range. Some payers approve a scan only for a specific imaging center. Some approvals expire after a short time. Staff should check these details before the patient arrives.
Need Help With Accurate MRI Billing?
Contact MedicalBilling.help today and make your MRI billing process easier.
Common MRI Claim Denials
MRI denials often happen because the payer finds a mismatch. The claim may show the wrong body area, wrong contrast use, wrong diagnosis, missing approval, or a service that does not match payer policy.
Another common denial happens when the claim uses a weak diagnosis. The diagnosis should come from the medical record. Staff should not guess or choose a code only to get payment. The claim must reflect the real reason for the scan.
Some denials happen when the payer asks for records and the practice sends incomplete notes. The appeal should include the order, final report, prior approval if available, clinical notes, and any test results that support medical need.
A good billing team tracks denial reasons each month. If one payer keeps denying the same MRI service, the team should review that payer policy and train staff on the issue.
Documentation Tips for Clean MRI Billing
Good documentation starts with the order. The order should show the body part, reason for the scan, contrast request, and ordering provider details. If the order is unclear, staff should ask for a clearer order before the scan.
The final MRI report should support the code billed. It should name the exam and show the body area. It should state contrast use clearly. It should include findings and an impression.
The provider note should support medical need. For pain cases, the note may need to show how long the pain has lasted, what treatment failed, and whether the patient has nerve signs. For cancer cases, the note should show the cancer history or reason for follow up.
The billing team should compare the report to the claim before submission. This small step can prevent many denials.
Best Practice Workflow for MRI Billing Teams
A strong MRI billing workflow starts before the appointment. The team should review the order, check benefits, verify prior approval rules, and confirm the correct imaging site.
On the scan date, the imaging team should document the service clearly. If the exam changes, staff should update the record. For example, if the patient cannot receive contrast, the report and claim should show the service that actually happened.
After the report is ready, the coder should choose the code from the final report. The claim team should check payer approval, diagnosis support, modifiers when needed, and provider details.
After payment or denial, the billing team should review the result. Paid claims show what worked. Denied claims show where the process needs improvement.
Why Accurate MRI Coding Helps Your Practice
Accurate MRI coding helps the practice get paid faster. It also reduces rework, phone calls, appeals, and patient billing confusion. When the code matches the report, the payer has less reason to stop the claim.
Accurate coding also protects the practice during audits. Payers may ask for records after payment. If the documentation supports the MRI CPT Codes billed, the practice can respond with confidence.
Patients also benefit from clean billing. They receive clearer statements, fewer corrected claims, and fewer surprise balance changes. This builds trust between the patient and the provider office.
Key Takeaway for MRI CPT Codes
MRI CPT Codes are important for clean claims and fair payment. The right code depends on the body area, contrast use, exam type, and final report. Billers should never guess from the schedule alone.
A clean MRI claim needs clear documentation, correct diagnosis support, prior approval when required, and a code that matches the report. When the billing team follows these steps, the practice can reduce denials and improve cash flow.
MRI coding can feel hard at first, but most claims follow a simple process. Check the body area. Check contrast use. Read the report. Match the diagnosis. Confirm payer rules. Then submit the claim with confidence.
FAQ
What are MRI CPT Codes?
MRI CPT Codes are five digit billing codes that describe MRI imaging services. They tell the payer what body part was scanned and whether contrast was used.
What is the CPT code for MRI brain without contrast?
The common CPT code for MRI brain without contrast is 70551. The report should confirm that the provider did not use contrast.
What is the CPT code for MRI brain with contrast?
The common CPT code for MRI brain with contrast is 70552. The report should show that contrast was used.
What is the CPT code for MRI brain without and with contrast?
The common CPT code for MRI brain without and with contrast is 70553. The report should show images before and after contrast.
What is the CPT code for MRI lumbar spine without contrast?
The common CPT code for MRI lumbar spine without contrast is 72148. This code appears often in low back pain and spine care claims.
What is the CPT code for MRI cervical spine without contrast?
The common CPT code for MRI cervical spine without contrast is 72141. This code applies to the neck part of the spine.
Why does contrast change MRI CPT Codes?
Contrast changes the MRI service because the provider uses contrast material to get more image detail. Many MRI areas have separate codes for without contrast, with contrast, and without and with contrast.
Do MRI claims need prior authorization?
Many payers require prior authorization for MRI claims. The billing team should check payer rules before the scan date.
Are MRI and MRA codes the same?
No. MRI and MRA codes are different. MRI looks at body structures. MRA focuses on blood vessels.
What causes MRI claim denials?
Common denial causes include missing prior approval, wrong contrast code, weak diagnosis support, wrong body area, and payer policy issues.
How often should billing teams update MRI CPT Codes?
Billing teams should review MRI CPT Codes every year and check payer updates during the year. CPT and payer rules can change.




