If you are working in healthcare billing or planning to start, you must understand how to calculate allowed amount in medical billing. This concept plays a major role in how providers receive payments and how patient balances are calculated. Many beginners find it confusing at first, but once you understand the logic, it becomes very simple and practical.
In medical billing, the amount a provider charges is not always what they receive. Insurance companies follow their own pricing rules, and that is where the allowed amount comes in. This is the amount that insurance agrees to pay for a service, and everything else is adjusted or passed to the patient based on their plan.
Understanding this concept will help you read claims correctly, avoid mistakes, and improve billing accuracy.
Table of Contents
ToggleWhat Is Allowed Amount in Medical Billing
The allowed amount is the maximum amount an insurance company agrees to pay for a medical service. It is often lower than the billed amount because insurance companies have contracts with providers that define specific rates.
For example, a provider may charge 250 dollars for a service, but the insurance company may only allow 150 dollars. That 150 dollars becomes the allowed amount. This is the amount used to calculate payments and patient responsibility.
This is the core idea behind medical billing allowed amount, and it applies to almost every claim processed in the system.
Why Allowed Amount Is Important
The allowed amount directly affects how much the provider gets paid and how much the patient owes. It is not just a number, but the base for all financial calculations in a claim.
When you understand how insurance payments work, you can easily break down any claim. You can see how much the insurance paid, how much the patient owes, and how much is written off.
Without understanding the allowed amount, it becomes difficult to identify errors or underpayments. That is why this concept is essential for anyone working in billing.
Understanding the Difference allowed amount vs billed amount
One of the most common areas of confusion is the difference between allowed amount vs billed amount. The billed amount is what the provider charges, while the allowed amount is what the insurance approves.
The difference between these two amounts is usually written off. This means the provider cannot bill the patient for that portion if they are in network with the insurance company.
Once you clearly understand this difference between allowed amount vs billed amount, the rest of the billing process becomes much easier to follow.
How to Calculate Allowed Amount in Medical Billing
Now let us move to the main part of this guide. To calculate allowed amount in medical billing, you need to look at the claim details carefully.
Start by reviewing the Explanation of Benefits or EOB. This document shows how the insurance processed the claim. It includes the insurance payment and the patient responsibility.
The simplest way to calculate the allowed amount is by adding the insurance payment and the patient responsibility. This is the most reliable method when working with real claims.
This method is also based on the insurance allowed amount formula that billing professionals use every day.
Simple Example for Better Understanding
Let us take a real example to make things clear. Suppose a provider charges 300 dollars for a service. The insurance company reviews the claim and decides that the allowed amount is 180 dollars.
Out of this 180 dollars, the insurance pays 120 dollars. The remaining 60 dollars is the patient responsibility.
When you add 120 and 60, you get 180 dollars. That is your allowed amount. The remaining 120 dollars from the original billed amount is written off.
This example clearly shows how to calculate allowed amount in medical billing using real numbers.
Another Scenario You May See Often
Sometimes, the insurance does not pay anything because the patient has not met their deductible. In this case, the entire allowed amount becomes the patient responsibility.
For example, if the billed amount is 400 dollars and the allowed amount is 200 dollars, the patient may have to pay the full 200 dollars. The remaining 200 dollars is written off.
This situation is common and shows that the allowed amount is not always linked to insurance payment alone.
How Insurance Contracts Affect Allowed Amount
Insurance companies and providers sign contracts that define how much will be paid for each service. These contracts include fixed rates for different procedures.
The allowed amount is based on these contract rates. This is why different insurance companies may allow different amounts for the same service.
If you want to explore more about how these systems work, you can visit https://www.cms.gov which provides official healthcare billing guidelines.
Understanding contract rates helps you better calculate allowed amount in medical billing and detect payment issues.
Common Errors to Watch For
Many billing errors happen because people misunderstand the allowed amount. Some assume that the billed amount is the same as the allowed amount, which is not correct.
Others forget to include patient responsibility in their calculation. This leads to incorrect totals and confusion.
Always check the EOB carefully and make sure you include both insurance payment and patient responsibility when calculating the allowed amount.
Why This Skill Matters in Your Career
Learning how to calculate allowed amount in medical billing can improve your accuracy and confidence. It helps you understand claims clearly and communicate better with insurance companies.
It also helps you identify underpayments and ensure that providers receive the correct reimbursement.
Whether you are new or experienced, this skill is essential for success in medical billing.
Mastering Allowed Amount in Medical Billing
The allowed amount is one of the most important parts of medical billing. It defines how payments are calculated and how much the patient is responsible for.
Once you understand how to calculate allowed amount in medical billing, you will find it much easier to work with claims and resolve billing issues.
Practice with real examples, review EOBs regularly, and keep learning. Over time, this process will become natural and easy for you.
How Allowed Amount Is Calculated by Insurance Companies
To fully understand how to calculate allowed amount in medical billing, it is important to know how insurance companies decide this amount in the first place.
Insurance companies do not randomly assign values. They follow structured pricing models based on contracts, regional data, and standard fee schedules. These schedules are created after analyzing healthcare costs, provider agreements, and market rates.
Most insurance companies rely on negotiated contracts with providers. These contracts define how much will be paid for each service code. In many cases, these rates are lower than the provider’s billed charges.
In addition, some insurers use benchmarking systems such as usual and customary rates. These rates are based on what similar providers charge in a specific area. This method is often used for out of network claims.
Understanding this process helps you better interpret the insurance allowed amount formula and identify whether payments are correct or not.
Components That Make Up the Allowed Amount
The allowed amount is not a random number. It is made up of different financial components that together form the total approved amount.
When you calculate allowed amount in medical billing, you are actually combining different parts of a claim. These include the insurance payment and the patient responsibility.
The patient responsibility itself may include deductible, copay, and coinsurance. Each of these elements depends on the patient’s insurance plan.
When you understand these components clearly, you can easily break down any claim and see how insurance payments work in real situations.
Confused About Allowed Amount Calculations?
Discover how to break down insurance payments and ensure accurate billing every time.
Table Example of Allowed Amount Calculation
Here is a simple table to help you visualize how the allowed amount is calculated in a real claim scenario.
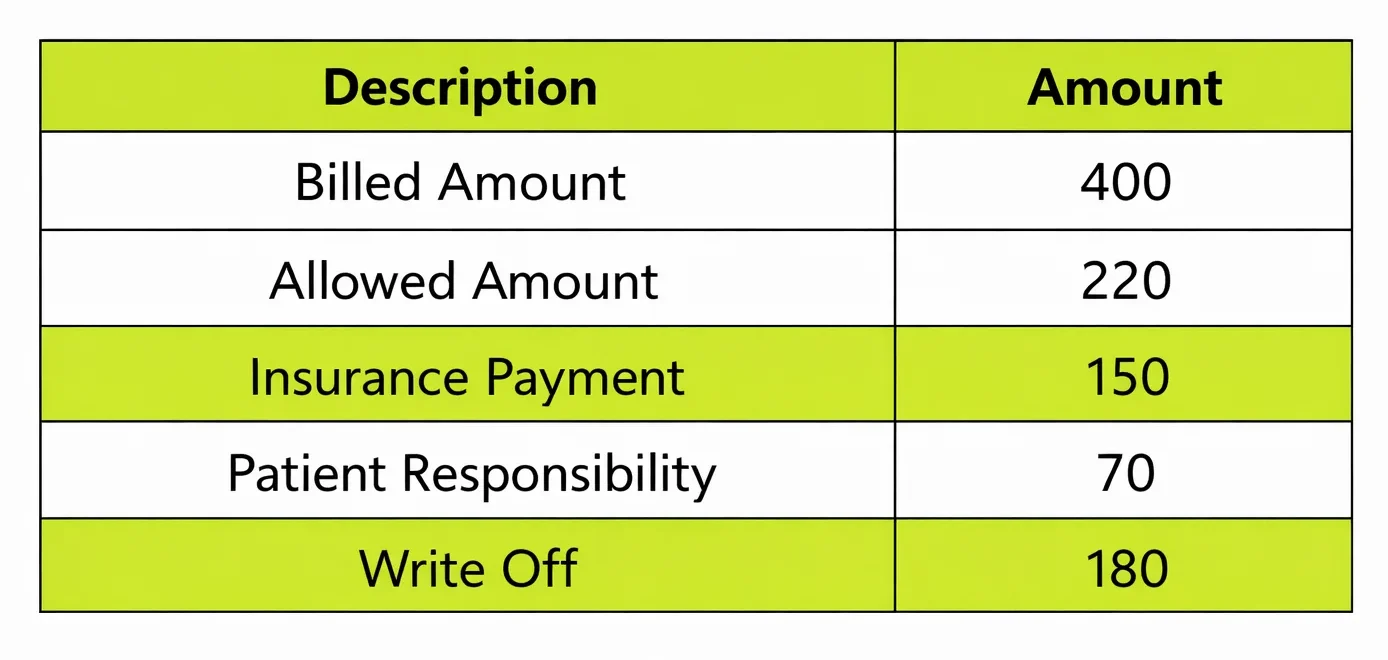
In this example, the provider billed 400. The insurance allowed only 220. Out of this, 150 was paid by insurance and 70 was assigned to the patient.
The remaining 180 is written off. This clearly shows the difference between allowed amount vs billed amount and how each part plays a role.
Role of EOB in Calculating Allowed Amount
The Explanation of Benefits is one of the most important documents in medical billing. It gives a detailed breakdown of how a claim was processed.
When you want to calculate allowed amount in medical billing, the EOB is your main reference. It shows the billed amount, allowed amount, insurance payment, and patient responsibility.
You should always review the EOB carefully because it also includes adjustment codes and remarks that explain why certain amounts were reduced or denied.
By reading the EOB regularly, you can improve your accuracy and avoid common billing errors.
Difference Between In Network and Out of Network Allowed Amount
The allowed amount can change depending on whether the provider is in network or out of network.
In network providers have agreements with insurance companies. They must accept the allowed amount as full payment and cannot charge the patient extra beyond their responsibility.
Out of network providers do not have such agreements. In these cases, the insurance company may allow a lower amount, and the provider may bill the patient for the remaining balance.
This is why understanding network status is important when learning how to calculate allowed amount in medical billing.
How Allowed Amount Impacts Revenue Cycle Management
The allowed amount plays a central role in revenue cycle management. It directly affects how much a healthcare provider earns from each service.
If the allowed amount is calculated incorrectly or not verified, it can lead to underpayments and revenue loss. Billing teams must review claims carefully to ensure accuracy.
By understanding medical billing allowed amount, billing professionals can identify discrepancies, follow up with insurance companies, and improve overall financial performance.
How to Identify Underpayments Using Allowed Amount
One of the biggest advantages of knowing how to calculate allowed amount in medical billing is the ability to detect underpayments.
If the insurance payment plus patient responsibility does not match the expected allowed amount based on the contract, it may indicate an error.
In such cases, you can compare the claim with the contract rate and raise an appeal if needed.
This process helps ensure that providers receive the correct reimbursement for their services.
Advanced Scenario with Multiple Procedures
In real life, claims often include multiple procedures. Each procedure may have a different allowed amount.
For example, a claim may include two services with different CPT codes. Each code will have its own allowed amount based on the contract.
You must calculate the allowed amount for each procedure separately and then combine them to get the total allowed amount for the claim.
This makes the process slightly more complex, but the basic concept remains the same.
How Technology Helps in Allowed Amount Calculation
Modern billing software can automatically calculate allowed amounts based on claim data and insurance rules.
However, relying only on software is not enough. You should always understand the logic behind the calculation so you can verify results and catch errors.
Technology improves speed, but knowledge ensures accuracy.
Common Questions Patients Ask About Allowed Amount
Patients often get confused when they receive medical bills. They usually expect insurance to pay the full billed amount.
When they see a lower payment, they may question why they still owe money. This is where understanding allowed amount becomes important.
You can explain to patients that insurance only pays the approved amount, not the full charge. This helps build trust and reduces confusion.
FAQ
What is allowed amount in medical billing
The allowed amount is the maximum amount an insurance company will pay for a covered service. It is also called the negotiated rate or eligible expense.
How to calculate allowed amount in medical billing
You calculate the allowed amount by adding the insurance payment and the patient responsibility. This includes deductible, copay, and coinsurance.
Is allowed amount the same as billed amount
No, the billed amount is what the provider charges, while the allowed amount is what the insurance approves. The difference is usually written off.
Why is the allowed amount lower than the billed amount
Insurance companies use contract rates or fee schedules, which are lower than provider charges. This creates a difference that is written off.
Who decides the allowed amount?
The insurance company decides the allowed amount based on contracts, fee schedules, or usual rates. It can vary between plans and providers.
What is the difference between allowed amount and insurance payment
The allowed amount is the total approved amount, while the insurance payment is only a portion of it. The rest is paid by the patient.
Does patient responsibility come from the allowed amount
Yes, patient responsibility such as deductible and coinsurance is always calculated from the allowed amount, not the billed charge.
What happens if the billed amount is higher than allowed amount?
If the provider is in network, the extra amount is written off. If the provider is out of network, the patient may have to pay the difference.
Can allowed amount be different for the same procedure
Yes, different insurance companies and plans have different allowed amounts for the same service due to different contracts.
What is contractual adjustment in medical billing
Contractual adjustment is the difference between the billed amount and the allowed amount. This amount is written off and cannot be charged to the patient in most cases.
How does deductible affect allowed amount
If the patient has not met the deductible, they may have to pay the full allowed amount before insurance starts paying.
What is coinsurance based on allowed amount
Coinsurance is a percentage of the allowed amount that the patient must pay after meeting the deductible.
Is allowed amount the final payment to the provider
No, the allowed amount is the total approved amount. The provider receives part from insurance and part from the patient.
Where can I find the allowed amount on a claim
You can find the allowed amount on the Explanation of Benefits or Electronic Remittance Advice, where all payment details are listed.
Can allowed amount be zero
Yes, if the service is not covered or denied, the allowed amount may be zero.
How do in network and out of network affect allowed amount
In network providers must accept the allowed amount as full payment, while out of network providers may charge the patient extra.
What role do CPT codes play in allowed amount
CPT codes help insurance companies determine the allowed amount because each code has a specific rate in the fee schedule.
Does allowed amount change every year
Yes, allowed amounts can change based on updated contracts, fee schedules, and policy changes.




